Nudy M, et al. The severity of vasomotor symptoms and number of menopausal symptoms in postmenopausal women and select clinical health outcomes in the Women’s Health Initiative Calcium and Vitamin D Randomized Clinical Trial. Presented at: North American Menopause Society Annual Meeting; Sept. 28, 2020 (virtual meeting).
Nudy reports no relevant financial disclosures.
ADD TOPIC TO EMAIL ALERTS
ADDED TO EMAIL ALERTS
Women who reported two or more moderate to severe menopause symptoms had increased risks for cardiovascular disease and stroke, but vasomotor symptom severity did not affect risk, according to data from the WHI Calcium and Vitamin D trial.
“The severity of vasomotor symptoms was not associated with any clinical health outcome, and randomization to calcium and vitamin D did not change that,” Matthew Nudy, MD, cardiology fellow at Penn State Heart and Vascular Institute in Hershey, Pennsylvania, told Healio. “Having two or more moderate/severe menopausal symptoms was associated with increased CVD and stroke. Randomization to calcium and vitamin D did not alter this finding. The severity of many individual menopausal symptoms other than the core vasomotor symptoms was associated with total CVD.”
Nudy and colleagues presented the findings at the North American Menopause Society virtual meeting.
Researchers analyzed data collected during the Women’s Health Initiative-Calcium and Vitamin D trial (n = 20,050), a double-blind, randomized, placebo-controlled study in which women aged 50 to 79 years received 400 IU of 25-hydroxyvitamin D and 1,000 mg of elemental calcium per day, with researchers analyzing the effect of the supplements on health outcomes.
Participants self-reported menopause symptoms, including vasomotor symptoms, such as hot flashes and night sweats. Other menopause symptoms reported were dizziness, heart racing, tremors, feeling restless, feeling tired, difficulty concentrating, forgetfulness, mood swings, vaginal dryness, breast tenderness, headaches and waking up several times at night. Severity of symptoms was assessed at baseline with a questionnaire. Researchers examined occurrences of CVD, stroke, hip fracture, colorectal cancer, invasive breast cancer, all-cause mortality, coronary heart disease and a global index that included hip fracture, cancer and death outcomes (median follow-up, 7 years).
The data showed no association between severity of vasomotor symptoms and any health outcomes included in the trial. However, women who reported two or more menopause symptoms were at a higher risk for total CVD (HR = 1.35, 95% CI, 1.18-1.54; P < .001) and stroke (HR = 1.4, 95% CI, 1.04-1.89, P = .03) compared with women with no symptoms. Women who reported one menopause symptom also had an elevated risk for stroke (HR = 1.2; 95% CI, 0.88-1.63; P = .03) compared with women with no symptoms.
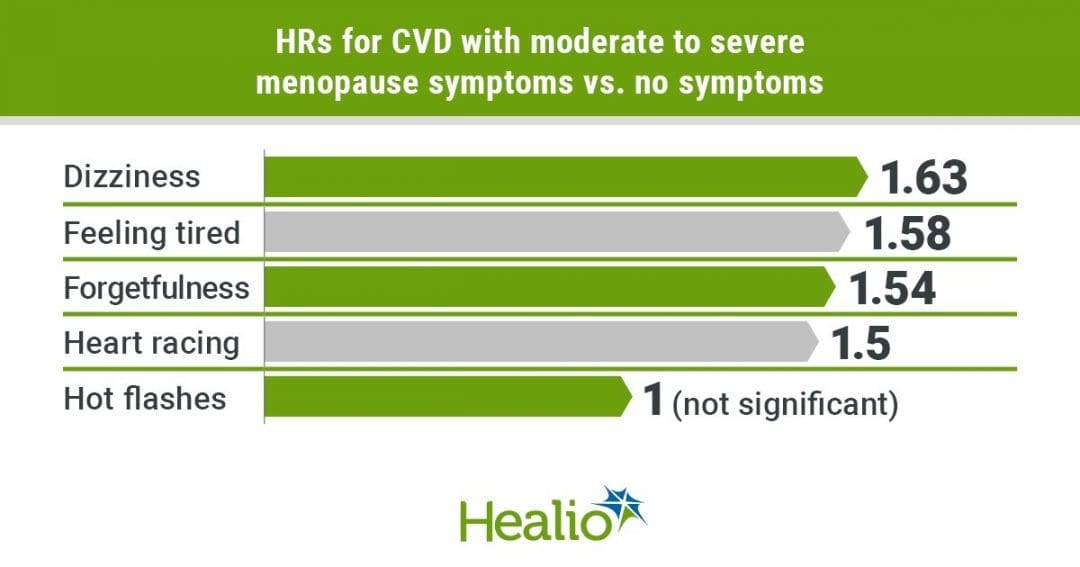
Participants who reported moderate or severe symptoms of dizziness (HR = 1.63; 95% CI, 1.31-2.04; P < .001), heart racing (HR = 1.5; 95% CI, 1.23-1.83; P < .001), restlessness (HR = 1.36; 95% CI, 1.13-1.65; P = .02), feeling tired (HR = 1.58; 95% CI, 1.31-1.91; P < .001), difficulty concentrating (HR = 1.34; 95% CI, 1.08-1.66; P = .01), forgetfulness (HR = 1.54; 95% CI, 1.31-1.8; P < .001) and headaches or migraines (HR = 1.2; 95% CI, 1.02-1.4; P = .008) were at higher risk for total CVD. The associations did not change after adjusting for the calcium and vitamin D supplement in the trial.
“More moderate and severe menopausal symptoms are associated with increased cardiovascular disease and stroke,” Nudy said. “These patients may be more likely to seek a physician for treatment, and this may be an ideal time to assess cardiovascular disease risk.”
Nudy added that future research should examine individual menopause symptoms to determine which are associated with the highest CVD risk.
Holly L. Thacker MD, FACP, CCD, NCMP
This study reinforces that women with moderate to severe menopausal symptoms need medical evaluation and treatment, and women with more moderate to severe menopausal symptoms have higher risks of cardiovascular disease and stroke. Not surprising, randomization to calcium and vitamin D did not mitigate those symptoms or increased cardiovascular risk.
All midlife women deserve cardiac risk assessment, which is the No. 1 cause of death; however, those women with more intense symptoms may be at more risk due to hormonal deficiency. Women who have palpitations, hypertension and other cardiovascular symptoms still deserve cardiovascular work up, but many times do better when treated with hormone therapy.
Midlife is an excellent time to assess not only cardiovascular risk, but osteoporosis risk, breast cancer risk and general health habits.
The “global index” was not a validated instrument, and as such, clinically, that’s much less helpful than the long-term data we have that show that women treated with menopausal hormone therapy within 10 years of menopause and for 5 or more years live longer!
In 2020, there is no excuse to not evaluate and treat symptomatic women, and for most women, the benefits of hormone therapy outweigh risks.
ADDED TO EMAIL ALERTS
This content was originally published here.