Also known as surgical menopause, hysterectomy is the surgical removal of the uterus. In most cases, menopause is natural. In the United States, the average menopausal age is 52. As the average woman gets to her mid-ages, the ovaries gradually lose the ability to produce eggs, leading to the inability to get pregnant naturally. While menopause happens mostly during the 50s, hysterectomy can lead to menopause at any age.
Understanding Menopause
Menopause is characterized by ovarian failure. As you get older, the functionality of your ovaries reduces. It is easier for a 33-year-old woman to get pregnant than a woman in her 40s. As you approach your 50s, your ovaries shrink to the extent that it stops producing viable eggs. With unviable eggs being produced, pregnancy becomes extra difficult, and on getting to Menopause, the ovaries completely lose the ability to produce eggs. During menopause, natural pregnancy is impossible.
Besides being producers of eggs, the ovaries are the main source of major sex hormones like estrogen and progesterone. On getting to menopause, the ovaries do not just lose the ability to produce eggs; they also, in most cases, decrease their ability to produce some of these sex hormones. With the decline in hormone production, menopausal women are more at risk of estrogen and progesterone decline. As mild as this problem may seem, it is important to know that a decline in hormone levels causes most menopausal symptoms experienced by women today.
Many people see menopause as an all-natural phase of life. However, menopause can also be triggered by non-natural causes. A woman automatically gets into menopause when she loses the ability to get pregnant. Whether natural ovarian failure or loss of child-bearing abilities by artificial causes, a woman is considered menopausal once she becomes unable to reproduce.
Understanding Hysterectomy
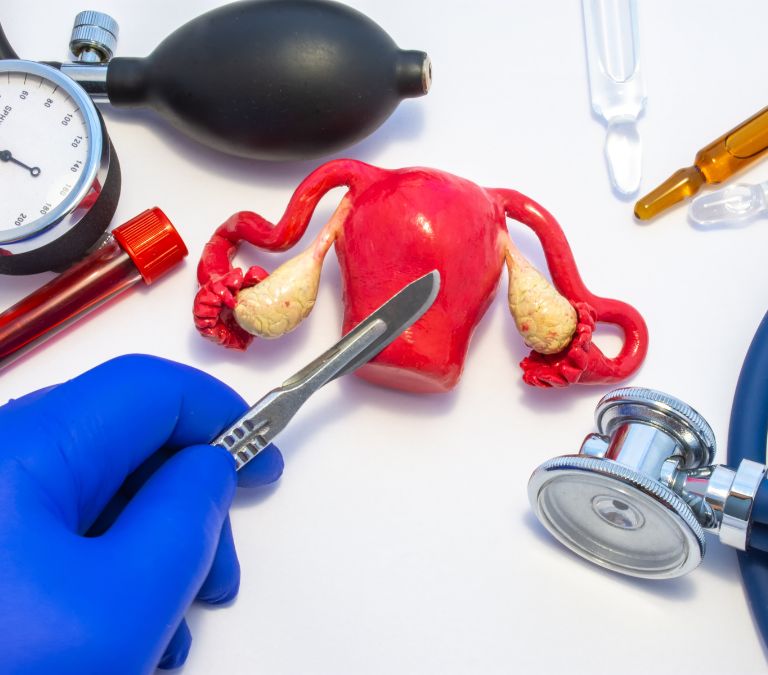
Hysterectomy is the surgical removal of the uterus. With hysterectomy, you will no longer be able to reproduce, and as such, you are in menopause. Hysterectomy may also involve the removal of the ovaries, fallopian tubes, cervix, and other reproductive system structures.
Of all gynecological surgical procedures in the United States, Hysterectomy is the second most performed, just after cesarean section. A gynecologist performs a hysterectomy and is only recommended when there aren’t other options. More women are opting for hysterectomy, which has increased its popularity significantly.
Reasons for Hysterectomy
There are many reasons for hysterectomy, the most common being fibroid and cancer. More than half a million hysterectomy procedures are performed yearly, and they come for different reasons. Generally, most women do not fancy the idea of artificial menopause. For non-menopausal women, hysterectomy can be emotionally difficult because pregnancy becomes impossible after the surgery.
In many cases, the woman still has plans to bear kids, and the idea of jeopardizing this can be tough to handle. However, hysterectomy procedures are only recommended when other procedures are not feasible enough and are a matter of life and death. While hysterectomy can be difficult for many women, it is important to know that it is only done to solve a life-threatening problem. Here are the most common reasons for hysterectomy:
Fibroids
Fibroids are benign growths in the womb and surrounding regions. They are non-cancerous and are very popular in women, especially women still in their reproductive years. Although women with fibroids do not typically show symptoms, some women have reported symptoms like heavy or painful periods, constipation, lower back pain, and painful intercourse.
The cause of fibroids hasn’t been comprehensively uncovered. However, research has linked fibroid development to the estrogen hormone. Fibroids typically shrink after menopause, but fibroids may cause severe bleeding during years of reproduction, which may warrant a hysterectomy. While fibroids do not often require treatment, some cases might produce worrying symptoms that an invasive surgery like a hysterectomy is needed.
A hysterectomy can be your best option if you have large fibroids and do not want more kids.
Heavy Periods
Every month, the ovaries produce an egg to be fertilized. With the release of eggs from the ovaries, hormones cause the buildup of a lining in the walls of the uterus. The lining now created in the uterus will house and develop the egg if fertilized. When the egg is released by the ovaries but not fertilized, the lining already created by the actions of the hormones begins to break down, and this causes the monthly bleeding from the vagina.
Periods typically last for three days; during this process, the body loses about three tablespoons of blood. In some cases, periods can last for up to seven days with the release of more than 9 teaspoons of blood. When periods come like this, it is known as menorrhagia or heavy periods.
Women who experience heavy periods are more likely to experience severe pains and stomach cramps. In many cases, heavy periods are caused by fibroids. However, the cause of many cases of heavy bleeding hasn’t been identified.
There are several treatment options for heavy periods, but hysterectomy may be the only way in cases where these treatments do not work. Hysterectomy can significantly impact the quality of life of many women, and if these women do not wish to have children, hysterectomy is performed.
Pelvic Inflammatory Disease
The reproductive system of women is more prone to infections when compared to that of men. Pelvic inflammatory disease is just one of those infections specific to the female reproductive system. Also known as PID, pelvic inflammatory disease is a bacterial infection that most often occurs from the transfer or spread of sexually transmitted bacteria from the vagina to the uterus.
The pelvic inflammatory disease often comes with mild, undetected symptoms until later. Many women living with the pelvic inflammatory disease do not even know of it; by the time they do, severe complications have already stepped in.
When detected early, you can treat pelvic inflammatory disease, but when it spreads, it can damage reproductive organs like the uterus and the fallopian tubes. PID causes severe pains, and a hysterectomy can be recommended when the pains become overwhelming. A hysterectomy procedure for PID removes the uterus and the fallopian tubes.
Endometriosis
Recall that during menstruation, certain hormones trigger the buildup of a lining in the walls of the uterus. Endometriosis is a condition that causes the buildup of lining in areas outside of the uterus. Just like the lining of the uterus, the lining now formed outside the uterus breaks down at the end of every menstrual cycle.
Generally, the lining of the uterus breaks down, and the blood flows out of the body via the vagina. When the lining outside the uterus breaks down, the blood will have nowhere to go, which may lead to swelling and inflammation of the surrounding areas. With this, scarring and lesions are formed in the tissues. Endometriosis can cause severe pains, irregular periods, and even fertility.
For endometriosis, hysterectomy is only performed when other treatment options have not effectively alleviated it. Hysterectomy for endometriosis removes the swollen areas that are usually important organs of the reproductive system. With this, the woman becomes unable to bear children anymore.
Adenomyosis
Adenomyosis is a condition that causes the endometrium to break through the muscle wall of the uterus. From boating to cramps and abdominal pain, adenomyosis, and heavy periods, adenomyosis can tamper with the standard of living of many women. Generally, adenomyosis doesn’t show any symptoms. However, it can cause severe menstrual cramps and bloat.
Adenomyosis is treated during mild cases. However, women showing significantly severe symptoms and who have no intentions of bearing children may be required to go for a hysterectomy.
Prolapse of the Uterus
When the muscles and ligaments supporting the uterus weaken, a prolapsed uterus may be formed. Due to the weakness of supporting muscles, the uterus may drop from its original position, and in many cases, the uterus slips down into the vagina. Women of all ages can have uterus prolapse, but it is more common in women at the later stages of menopause (postmenopause).
A prolapsed uterus is characterized by a sensation of heaviness in the pelvic region and a constant feeling of something being pulled out from your vagina. Other prolapsed uterus symptoms include urinary incontinence, slow bowel movement, back pain, and difficulty having sex.
Since a weakened pelvic floor muscle is the main cause of uterus prolapse, treatment of uterus prolapse is usually aimed at strengthening the pelvic floor muscles. Common causes of weakened pelvic floor muscles include pregnancy, obesity, delivery of a large baby, and low estrogen influenced by menopause.
Because hysterectomy involves the removal of the womb, it can be recommended as a permanent solution to uterus prolapse. Hysterectomy is best when the pelvic floor muscles are severely weakened and the woman has no plans of bearing children.
Cancer
In some cases, hysterectomy may be recommended for cancer treatment. Cancers like cervical cancer, cancer of the fallopian tubes, ovarian cancer, and cancer of the uterus may require hysterectomy when cancer has spread to an advanced stage. In most cases, hysterectomy is the only effective treatment and must be carried out as soon as possible.
The type of hysterectomy performed usually depends on the type or severity of the cancer. For endometrial cancer, a total hysterectomy is performed, and for cervical cancer, a radical hysterectomy is performed. Hysterectomy for cancer treatment often involves other cancer therapies like hormone therapy, radiation therapy, and chemotherapy.
Types of Hysterectomy
The reason for hysterectomy can influence the type of hysterectomy performed. A gynecologist may remove all or part of the uterus. While hysterectomy can be the only option in certain situations, removing just a part of the uterus could be the solution instead of removing all of it. The types of hysterectomy include;
Total Hysterectomy
In a total hysterectomy, the uterus, the cervix, the fallopian tubes, and one or both ovaries are removed.
Radical Hysterectomy
Radical hysterectomy involves the removal of the entire uterus, the cervix, part of the vagina, and other tissues of the uterus and cervix region. Radical hysterectomy is only done when cancer is present. Cancers like ovarian and cervical cancer are the most common reasons for a radical hysterectomy procedure. In some cases, the ovaries and fallopian tubes are also removed. If the ovaries aren’t removed, you still lose the ability to reproduce, but symptoms of early menopause are prevented.
After a radical hysterectomy, you permanently lose the ability to bear children, but your sexual function remains unaffected. Before having a radical hysterectomy, it is important to have a comprehensive discussion with a doctor, as it is considered a very big step and will most likely change your perspective of life.
Supracervical or subtotal hysterectomy
In a subtotal hysterectomy, the main body of the uterus is removed, but the cervix remains untouched. Subtotal hysterectomy is rarely done due to developing cervical cancer. The cervix serves as the neck of the uterus as it allows the passage of fluids from the vagina to the uterus and vice versa.
Since the cervix is not removed, it is possible to get pregnant, but it is impossible to carry the pregnancy because the uterus is non-existent. The ovaries can sometimes be removed, leading to the development of menopausal symptoms to prevent an ectopic pregnancy.
Deciding to have a Hysterectomy
For non-menopausal women, deciding to have a hysterectomy means kissing bye-bye to the ability to carry a child. Due to the magnitude of hysterectomy surgery, deciding to have one might be an extremely difficult task.
Anxiety is common before a hysterectomy procedure is performed, but with these steps, you can sure of good preparations on your way to getting optimal satisfaction from a hysterectomy;
Gathering Information
Most women who opt for hysterectomy are not well-informed on what it entails. While many women are well-informed on the inability to bear children after hysterectomy, the risks, menopausal symptoms, and other factors aren’t comprehensively discussed. Getting all the necessary information is important to feel confident and enlightened on the procedure. Talk directly to your doctor, not Siri, to get the information you need. Your doctor knows best; as such, you should ask questions and get clarity on hysterectomy before opting for it.
Following the Doctor’s Prescription
Before taking any medications, supplements, dietary options, or even lifestyle changes, ensure you get approval from your doctor. When administered with medicines and other substances, ensure you follow them and do not take any third-party substance without getting approval from your doctor. Hysterectomy is major surgery, and the things you do will make the process easier or more difficult.
Planning for Help
It could take several weeks to fully recover from a hysterectomy, and the recovery path can sometimes be tough and excruciating. Studies have shown that patients who get support are more likely to recover faster from an illness. Before a hysterectomy, ensure you have people to support you after the surgery. There should be people to help you do important things like driving, lifting heavy objects, and basically, help you with your day-to-day activities while you recover.
Risks of Hysterectomy
Hysterectomy is considered safe. However, all surgical procedures come with risks and complications. In rare cases, a typical hysterectomy procedure risks include infections, excessive bleeding, blood clots, early menopause, damage to the urinary tract, and death.
Aftermath of Hysterectomy
After a hysterectomy, pregnancy becomes impossible, and you are officially in menopause. as a menopausal woman, hormonal fluctuation is imminent, and you are more at risk of many conditions that, in many cases, can be severe.
The ovaries are the primary producers of estrogen hormones. Since most cases of hysterectomy involve the removal of the ovaries, estrogen levels go through an alarming decline which can trigger the development of symptoms known widely as “menopausal symptoms.”
Menopausal Symptoms after Hysterectomy
Many cases of women opting for hysterectomy are menopausal women. Since they are already in menopause, the surgical removal of the ovaries is not much of a big deal and will, in most cases, not cause severe health complications. However, non-menopausal women who engage in hysterectomy are more likely to experience severe menopausal symptoms.
To prevent the development of menopausal symptoms, the doctor tries as much as possible to ensure the ovaries are not removed. However, removing the ovaries may be extra important and, as such, has to be done. When the ovaries are removed, you not only lose the ability to reproduce; you also have an increased risk of several menopausal symptoms caused by a decline in hormones naturally produced by the ovaries.
With the ovaries gone and estrogen now in decline, menopausal symptoms may begin to step in. some common menopausal symptoms include hot flashes, night sweats, and sleep distortion. Some other menopausal symptoms include bloating, vaginal dryness, eye dryness, anxiety, depression, memory loss, brain fog, fatigue, hair loss, dry skin, vaginal itching, and low libido. Menopause also increases your risk of cardiovascular diseases, osteoporosis, weight gain, certain cancers, and urinary incontinence. Generally, menopause comes with many complications.
While menopause can come with its problems, many menopausal women go on to live healthy lives without many complications. However, some women experience the most severe symptoms that could cause significant impairment to their quality of life. However, innovations in medicine have provided options for effectively managing menopausal symptoms. With the right treatment and management options, you can go through a smooth transition into menopause with few complications.
Managing Menopausal Symptoms after Hysterectomy
While hysterectomy leads to artificial menopause, it is important to know that menopause is not a disease. Natural or artificial, every woman must go into menopause. Several treatments and management options have been available to ensure a smooth ride through menopause. Here are some of the best ways to manage menopause:
Hormone Therapy
Hormone therapy is the most common and effective way to manage menopausal symptoms. Since the loss of ovaries leads to the decline of vital sex hormones, hormone therapy aims to balance the hormones by injecting artificial hormones into the body. By injecting the body with highly-needed hormones, several menopausal symptoms can be well managed or, better still, prevented.
Usually, doctors prescribe hormone therapy to menopausal women within the shortest possible timeframe. Long-term use of hormone therapy has been proven by research to increase a woman’s vulnerability to diseases like breast cancer, heart problems, and cardiovascular disease. For this reason, it is important to talk to a doctor before opting for hormone therapy.
Fruits and Veggies
Due to the risks involved with hormone therapy, many women have sought effective alternatives for their menopausal problems. While hormone therapy remains the most effective treatment and management option for menopausal symptoms, studies have shown that several diet options could be effective enough to live healthy lives free of complications even in menopause.
Fruits and vegetables are of immense health benefit. Generally, studies have shown that fruits and greens are the healthiest diets for optimal health. Also, studies have shown that menopausal women who consume more fruits and greens are less likely to experience severe menopausal symptoms.
Fruits and vegetables contain high amounts of antioxidants, minerals, and other important nutrients, which studies have proven to help relieve hot flashes, and night sweats and even reduce your risks of cardiovascular diseases. Following the American dietary guidelines, it is recommended that up to 50 percent of your diet should include fruits and vegetables.
Exercises and Other Physical Activities
Studies have shown that sedentary women are more likely to experience menopausal symptoms of worrying or high severity. By actively engaging in exercise, women in menopause can prevent weight gain, which reduces the risks of developing cardiovascular diseases and type 2 diabetes. Exercise can also help prevent osteoporosis, endometrial, and breast cancer.
Generally, active exercises breed a healthy life and are important for women of all ages.
Conclusion
Most women prefer to experience natural menopause. However, certain health complications may warrant a hysterectomy, leading to menopause. After a hysterectomy, it becomes impossible to carry a baby, and this automatically kick-starts your menopausal journey.
Menopause is not a disease; it is a natural phase of life that every woman must go through. Hysterectomy or not, all women who wish to thrive on earth for a long time must go through menopause. Whether you do it because of an illness or perhaps just because you are tired of using contraceptives, hysterectomy is a big deal that should be discussed in length with a doctor before commencing it.







