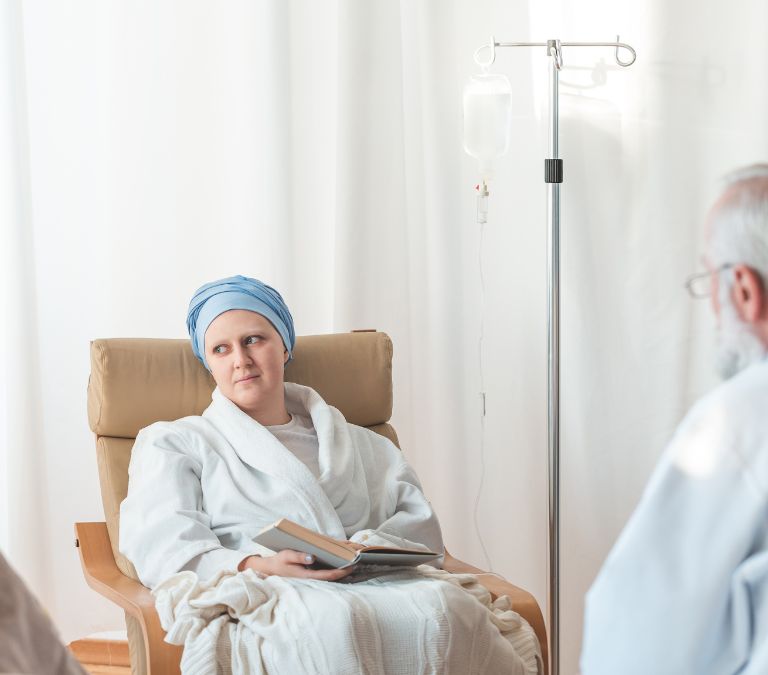
Menopause is something we all have to deal with as women. It is a natural phase of our lives that we must face as we age. When we reach menopause, we reach the end of our reproductive cycle. But we also face certain symptoms, like the debilitating heat stroke that almost sent me to my knees in the middle of the mall.
But menopause isn’t the only thing we have to deal with as we age. Age makes us susceptible to many conditions. Our heart becomes weaker, and our nervous system loses some of its function.
At the very top of this list of conditions is cancer. Your doctor might have already told you that your chances of getting breast cancer and other cancers increase as you go into menopause.
Does that mean these cancers are linked to menopause? Could this phase of our lives put us at risk of getting these diseases? Could the cancer treatment have anything to do with menopause? In this article, we will take a concise look at menopause, breast cancer, and chemotherapy; and their relationship with each other.
Menopause And Breast Cancer
Let’s tackle the elephant in the room. Does menopause put you at risk of breast cancer? There is no association between menopause and the risk of developing any cancer. Menopause is a normal phase we face as women; though it causes physiological and anatomical changes, it does not contribute to cancer risk.
However, the chances of cancer increase with age, so we can say that the chances of getting breast cancer during menopause are higher.
It is also likely that the treatment you are getting for your menopausal symptoms might increase your chances of getting breast cancer.
Hormone Replacement Therapy And Breast Cancer
I was reading a study that said the treatment for menopausal symptoms could increase or decrease your chances of getting cancer.
According to the study, prolonged exposure to female hormones puts you at risk of cancer. So just being a woman puts us at a disadvantage. But during menopause and in an attempt to treat our menopausal symptoms, we might turn to hormone replacement therapy (HRT).
The study I was reading postulated that the longer we are subjected to hormone replacement therapy in combination with progestin and estrogen as a treatment for menopausal symptoms, the higher our chances of getting breast cancer.
However, this does not mean you will get breast cancer just because you get hormone replacement therapy. Other factors might contribute to breast cancer. Have a detailed talk with your healthcare provider to ascertain your risk level and whether hormone replacement therapy would be a good option for treating your menopausal symptoms.
Menopause And Chemotherapy
Menopause seems to have another connection with cancer. We talked about how the treatment of menopausal symptoms can lead to cancer, but it also seems that cancer treatment can lead to early-onset menopause.
Chemotherapy is one of the most common cancer treatments. It uses powerful drugs to kill cancer cells. Cancer cells grow and multiply faster than most cells in the body, and the chemicals used in chemotherapy target these cells.
But chemotherapy does something else to women. It induces a condition known as chemo-induced menopause or chemopause. Chemopause is a condition where women who are not menopausal start showing signs of menopause while receiving chemotherapy.
It sounds confusing, right? I felt the same way too! If chemotherapy targets cancer cells, why is it inducing menopause? What is the relationship between chemotherapy and your reproductive physiology?
Menopause And Chemopause
We already know what menopause is. When you get to menopause, your reproductive cycle comes to an end. You can’t produce reproductive hormones, and your ovaries start to shrink and lose functionality. Because of these changes, your menstrual cycle will become irregular and eventually stop.
Menopause causes some temporary symptoms. The most common symptom is hot flashes. Hot flashes can range from mild to debilitating. Another very common symptom is insomnia. Because of the lack of sleep and hot flashes, menopausal women tend to be irritable.
When you have had this symptom for a year without having a complete menstrual cycle, you will be declared completely menopausal.
On the other hand, chemopause is a condition that people getting cancer treatment face. It is the early onset of menopause. Most people who suffer from chemopause present symptoms similar to those who are menopausal.
Hot flashes and night sweats are common in those with chemopause and can be more severe than menopausal symptoms. This begs the question, “why does chemotherapy induce these changes in us?”
How Does Chemotherapy Lead To Early Onset Menopause?
Chemotherapy is one of the most common treatments for cancer cases. It targets and kills cancer cells but isn’t as precise as we might like.
Chemotherapy doesn’t just target cancer cells. It is not that specific. It focuses on cells that proliferate quickly. The implication is that some healthy cells might be affected. These healthy cells killed by chemotherapy are the reason for some of the symptoms we see in people with cancer.
You lose your hair during chemo because the chemicals target the cells your body uses to produce hair.
Chemotherapy also affects your reproductive system. It affects your ovaries and throws your reproductive hormones off balance. Because of the changes to your cellular lifecycle and endocrine system, people getting chemotherapy might present with menopausal symptoms.
Not all women will experience this phenomenon. Some people undergo chemotherapy treatment without getting a single hot flash, while others get hot flashes so severe that they affect the quality of their lives.
Age is also an important factor here. You are more likely to get chemopause symptoms if you were already above 40 years when you started chemotherapy. This is because your hormone levels are declining, and the chemicals do not have to work as hard. But chemotherapy can also affect younger women.
Chemotherapy Medications That Might Lead To Chemopause
The most common chemotherapy medication that leads to menopause is cyclophosphamide. It is most commonly used in combination with methotrexate and fluorouracil. The combination is known as CMF.
Other chemotherapy combinations that can lead to menopause include:
- Cyclophosphamide, doxorubicin, fluorouracil (CAF)
- Doxorubicin and cyclophosphamide (AC)
- Cyclophosphamide, epirubicin, fluorouracil (CEF)
- Docetaxel, doxorubicin, and cyclophosphamide (TAC)
These are the most common chemotherapy combinations that lead to chemopause, but they are not the only ones. Ask your medical provider if the treatment regimen they want to use can induce menopause.
What Are The Symptoms Of Chemopause?
Chemocause is chemotherapy-induced menopause, so the symptoms are similar. Some of the most common symptoms are:
Vasomotor Symptoms
Like people with menopause, people with chemopause also present with vasomotor symptoms. They have hot flashes and night sweats. Like people with menopause, the severity of these symptoms varies from person to person, and not everyone gets them.
Insomnia
People with chemopause sometimes present with insomnia. Insomnia could be due to hormonal changes, or it could be due to night sweats. People with insomnia tend to be irritable and have mood swings, too, because of the lack of sleep.
Irregular Or No Menstrual Cycle
Chemopause also causes a change in the hormones responsible for menstrual periods. This is why women with chemopause tend to have irregular periods, which might eventually stop. In some cases, the normal menstrual cycle might resume after chemotherapy runs its course, but it could also be permanent.
Vaginal Discharge, Dryness, And Pain During Intercourse
Chemopause affects the reproductive hormones produced by the ovaries. These hormones do not just function as part of the reproductive cycle; they also affect the reproductive organs, like the vagina.
Because these hormones are no longer produced in the right amount, the vagina might become dry. This dryness could lead to inflammation, infection, and vaginal discharge. It could also cause pain during sexual intercourse.
Loss Of Libido
The pain during intercourse resulting from vaginal dryness will reduce interest in sex. Nobody wants to have sex if they are going to feel pain. The thought of pain will throw a wet towel on all thoughts about sex.
People with chemopause might also present with other menopausal symptoms like depression, anxiety, and weight gain. In some cases, the depression and anxiety might not be due to chemopause but because they face a life-altering situation.
How Do You Manage These Symptoms?
Chemopause is caused by chemotherapy; if chemotherapy is stopped, the symptoms might also disappear. But chemotherapy is a cancer treatment, and we cannot stop treating cancer because the consequences are more severe than menopausal symptoms.
But the fact remains that these symptoms can be debilitating, and as if cancer wasn’t difficult enough, you now have to deal with symptoms of chemopause.
Fortunately, you can manage symptoms of chemopause the same way you manage symptoms of menopause. However, there are some important differences:
- Hormone replacement therapy has to be monitored as some hormone replacement medications might increase the chances of cancer returning.
- Certain mood stabilizers should not be used during chemotherapy and while you are in remission.
Your healthcare provider is in the best situation to advise you on the actions to take and the best way to treat the symptoms of chemopause while you continue chemotherapy.
Hormone Replacement Therapy
Most people suffering from chemopause opt for HRT to help reduce their symptoms. Hormone medications that use progesterone and estrogen have shown amazing promise in treating chemotherapy-induced menopause.
But the use of HRT for managing chemopause is so complicated that you should properly discuss it with your healthcare provider before considering it. Whether this treatment option is good for you depends on factors like the type of cancer, your age, and the type of hormones used. If the doctor does not think hormone replacement therapy is a great idea, they will prescribe other treatment options.
Lifestyle Modifications
Sometimes, your symptoms are not severe enough to warrant medication. If this is the case, your doctor will most likely prescribe lifestyle modifications to reduce your symptoms. These lifestyle modifications are meant to reduce the triggers of your symptoms. Examples include
- Maintaining a healthy weight through regular exercise and a proper diet. Regular exercise can also help relax you and improve your mental health.
- Reduce the chances of hot flashes and night sweats by limiting the consumption of alcohol, spicy foods, and caffeine.
- If you are suffering from vaginal dryness and irritation, water-soluble lubricants are a great way to counter them and continue enjoying sexual intercourse.
- Wear light clothing and use light bedding to reduce the chances of any discomfort from hot flashes.
- Drink a lot of water to prevent vaginal infection, keep you hydrated, and prevent hot flashes.
Your doctor might also make diet modifications and give you some recommendations on other lifestyle modifications to make.
Nutritional Supplements
I once had a lengthy conversation with my friend who was combating some of her menopausal symptoms with nutritional supplements recommended by her doctor. It seems these nutritional supplements are also great for managing symptoms of chemopause.
Vitamin E in low doses might help reduce hot flashes and night sweats. Calcium supplements can help protect the bone from osteoporosis when taken with vitamin D.
Other supplements like black cohosh have anecdotes claiming the efficacy of their use in managing chemopause and menopausal symptoms. However, there is little or no scientific evidence showing such efficacy. If you want to try them because of these anecdotes and the numerous other health benefits they offer, ensure you get clearance from your healthcare provider.
You must also speak to your doctor before trying any dietary supplements because studies have shown that some of these supplements interact with chemotherapy and other cancer medications.
Alternative And Complementary Therapies
You might also want to try other forms of medicine. While dealing with some of my menopausal symptoms, I found that acupuncture was great for my hot flashes and helped me sleep better at night.
Aromatherapy also seemed to help me sleep better. Yoga helps with stress and anxiety. It relaxes you and is great for managing symptoms of chemopause and menopause.
However, do not overdo it, and do not forget to inform your healthcare provider of any alternative therapy you want to employ. If you want to try acupuncture, ensure you are using a licensed acupuncturist.
Other Medications
Apart from hormone replacement medications, there are other medications you can use to treat chemopause symptoms. Antidepressants have helped women with their hot flashes, with some seeing as much as a 61 percent decrease. Antidepressants are also great for mood swings, depression, and anxiety accompanying chemopause. The groups of antidepressants with the most success are Selective Serotonin Reuptake Inhibitors (SSRIs) and Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs)
Gabamentin, an anticonvulsant, is another nonhormonal medication that has shown promise in treating menopausal hot flashes.
These are serious medications that should not be used without the knowledge and consent of your healthcare provider.
Will You Still Have Chemo-induced Menopause After You Are Done With Chemotherapy?
I cannot give you a definite answer. Chemopause can be temporary or permanent. For some people, once they are done with chemotherapy, their menstrual cycle returns to normal and chemopause stops.
However, for others, chemopause continues even after therapy. No one knows for certain if their chemopause will be permanent or temporary, but your doctor should be able to make a guess based on the following information.
Your Age
The chances of your chemopause being permanent depends on how old you are when you start getting treatment. People above 45 years are highly likely to get permanent chemopause while undergoing chemotherapy.
While writing this article, I came across a study done in 2015. Two hundred fifty-five women who were not yet 45 years were treated with chemotherapy and had chemo-induced menopause. Out of the 255 participants, 84 had permanent chemopause, while the rest got their monthly periods several months after their treatment.
This shows that age might be an important factor, but a younger age does not guarantee that your chemopause will be temporary.
Type And Duration Of Chemotherapy
The type of chemotherapy you are getting might also influence whether your chemopause will be temporary or permanent. Your doctor will look at the type of cancer you have and the stage you are in and then prescribe a type of chemotherapy and the duration.
Depending on the type and duration, your chemotherapy might be temporary or permanent.
Your Hormone Levels Before Treatment
As we age, we start losing some of our endocrine functions, and our hormone levels start to decrease. Depending on how low your hormone levels were before you started chemotherapy, your menstrual period might or might not be permanent.
Other factors might contribute to whether your chemopause is permanent even after chemotherapy. Other treatment methods and strategies to conserve ovarian function might contribute to how long your chemopause lasts.
However, it seems age is the biggest contributing factor. People with temporary chemopause might notice that their periods are different. These people might also experience menopause faster than those who do not have chemopause.
What Are The Changes My Menstrual Flow Might Face After Chemopause?
Many women who have temporary chemopause notice changes in their menstrual cycle. Some women complain of irregular periods, while others say the number of days between periods increases.
Some women might have regular periods, but their flow will be different. Pay attention to your menstrual periods and stay in contact with your doctor. Report any bleeding that does not feel natural or is accompanied by other symptoms.
What Do I Do If I Want To Have Children After Chemotherapy?
For people who want to have children, the fact that there is a chance that chemotherapy might ruin this dream is enough to keep you awake at night. But there are ways to increase the chances of giving birth to children after chemotherapy, even if you have permanent chemotherapy-induced menopause.
One way is to freeze your eggs before treatment. You can use them for IVF and surrogacy when you want to have children.
Another option is to try medications that will cause your period to cease even before you start chemotherapy. Using this method preserves your ovaries and protects your eggs during chemotherapy.
Is It Possible To Conceive During Chemotherapy?
Not every woman experiences chemopause during pregnancy. And even though chemotherapy might induce menopause, it might not completely shut down your reproductive system. You can’t even be sure that your menstrual cycle has ceased because chemotherapy leads to irregular cycles. Your body could start a surprise cycle, and you wouldn’t be able to tell.
It is possible for women who still get their periods to have children during chemotherapy. But this isn’t a great idea because pregnancy during chemotherapy could lead to complications. Your treatment will take a toll on your body and affect the baby’s development.
To prevent these, you must always use quality birth control methods. However, if you notice signs of pregnancy, contact your healthcare provider immediately so that actions can be taken to reduce the effects of the treatment on you and the baby.
What Are Some Safe Birth Control For Women Undergoing Chemotherapy?
You should always use a barrier contraceptive during sexual intercourse, but these are not 100 percent effective. You can also use oral contraceptives; however, ensure you get approval from your healthcare provider because birth control pills may negatively affect those with breast cancer.
Whatever method of birth control you use should be safe and approved by your doctor before use.
Can I Get Pregnant After Chemotherapy?
It is not uncommon for women to want to get pregnant after chemotherapy. It is possible, and many women have successfully pulled it off. However, careful planning is necessary. If you have successfully completed your treatment, contact your oncologist and tell them about your plans.
There are not many cases where pregnancy led to cancer return; however, it should be considered with caution.
You might be worried about the risks of chromosomal or genetic defects in your child, but every doctor will tell you that there is no risk as long as you have completed your treatment before getting pregnant.
Are There Other Cancer Treatments That Can Lead To Menopause?
At this point, you might wonder if other cancer treatment options do not come with the risk of early onset treatment-induced menopause.
Depending on your cancer type, other treatment types can also lead to early-onset menopause. Some of these other treatment options include:
- Radiotherapy or Radiation therapy
- Hormone therapy
- Ovarian Shutdown
- Surgical removal of the ovaries when the cancer is in the ovaries.
All these treatment options can lead to treatment-induced menopause. So talk to your healthcare provider and follow their advice on the prescribed treatment.
Radiation Therapy
Radiation therapy can lead to early onset menopause or premature ovarian insufficiency in cases where the patient is below 40 years old. Radiation is toxic to the ovaries, and because it is used in high doses when treating cancer, there is every likelihood that you will suffer from early-onset menopause.
Like chemopause, the loss of your period due to radiation might be temporary or permanent. If it is temporary, you should start seeing your cycle within a year after radiation. However, recovering your menstrual cycle does not mean your fertility returns.
Radiation might cause your eggs to stop maturing, so they won’t be able to develop to the point where they can be fertilized.
Ovarian Shutdown
People with certain types of breast cancer might require treatment plans that shut down the ovaries, preventing them from producing estrogen. This temporary shutdown is also known as ovarian suppression.
Heightened estrogen levels aid the proliferation of breast cancer cells, so by shutting down the ovary’s ability to make this hormone, you help treat breast cancer and prevent a recurrence.
Ovarian shutdown requires medications known as luteinizing hormone-releasing hormone agonists. These drugs signal the brain to prevent the ovaries from producing estrogen. The most common agonists used are:
- Goserelin
- Leuprolide
The drugs are injections and should be administered once a month over several months. When your body stops producing estrogen, you will feel some symptoms of menopause. However, it is not permanent. When you stop taking the medications, your ovaries will slowly return to optimal function. If you are advanced in age, your ovaries might not return to full functionality again as you slowly go into menopause.
Ovarian shutdown does not mean you cannot get pregnant, either. Some women have gotten pregnant during an ovarian shutdown. If you have a male partner and are sexually active, ensure you get birth control to prevent complicated pregnancies.
Hormone Therapy For Breast Cancer
Breast cancers come in different forms. There are cancer cells that have an affinity for estrogen and progesterone. These cells depend on these hormones to grow, so a good way to stop the proliferation is to prevent these cells from attaching to these hormones.
Hormone therapy is a complementary treatment used after surgery to reduce the risk of cancer reoccurring. The treatment lasts five years and is great for women with hormone receptor-positive cancers.
The drugs used for this treatment can lead to early-onset menopause. They induce some of the most common symptoms of menopause, including irregular cycles, hot flashes, night sweats, and vaginal dryness. Some drugs used in this therapy might also cause some side effects. The most common are stress, headache, nausea, and bone pain.
The changes in your cycle during this treatment period are not permanent and should return to normal after treatment is over.
Surgical Removal Of The Ovaries
This is usually the last resort for women at risk of developing ovarian cancer or recurrent breast cancer. People with a family history of these cancers or who have tested positive for the BRCA1 or BRCA2 genetic abnormality might also need to remove their ovaries to prevent cancer.
Ovary removal, also known as oophorectomy, is the surgical removal of the ovaries and fallopian tubes. The removal of your ovaries will induce quick and permanent menopause. The side effects are also more powerful because, during normal menopause, your ovaries slowly lose their function, but in ovarian removal, your body suffers an immediate loss of function.
Your doctor will most likely prescribe treatment options to help reduce the symptoms until your body gets used to it.
8 Facts You Should Know About Menopause, Chemotherapy, And Cancer
Chemotherapy Can Lead To Temporary Or Permanent Menopause
Chemotherapy works by attacking cells that are proliferating quickly. The downside is that they can also attack the cells of the ovaries. This will cause the ovaries to stop processing mature eggs leading to temporary or permanent menopause in some cases.
In temporary cases, the menstrual cycle usually returns before two years. However, women who get temporary menopause during chemotherapy might also get complete menopause earlier than other women.
Whether the menopause caused by chemotherapy is temporary or permanent depends on the woman’s age. If you are above 45, the chances of your chemo-induced menopause being permanent is higher.
Treatment-induced Menopause Is Usually More Intense
Menopause is usually a slow process that might take a few years. However, cancer treatments expedite this process. Using some of the chemotherapy combinations mentioned above can induce menopause for months.
Because your body has not gotten used to this state, you will feel the symptoms of menopause more intensely. Younger patients might feel even more intense symptoms because they still have high hormone levels.
However, this isn’t always the case. Just like normal menopause, the severity of treatment-induced menopause will vary from person to person depending on factors such as age, lifestyle, and health history.
Temporary Treatment-induced Menopause Can Preserve Fertility
Even if you are getting cancer treatment, there is still a chance that you want to have children after your treatment.
If you are young enough, temporary menopause might just be advantageous, especially if you induce it before chemotherapy.
Think of it this way, you bought a pack of meat to make dinner, but then your friends invite you for a night out in town. To prevent the meat from going bad, store it in the refrigerator until you want to use it again.
When you induce menopause before starting chemotherapy, you are putting your eggs in a similar situation so that they are not harmed during chemotherapy, and your fertility remains the same afterward.
Your Lifestyle Might Reduce Or Increase Menopausal Symptoms
The intensity of the menopause symptoms you feel during chemotherapy might be due to your lifestyle.
An unhealthy lifestyle will worsen your menopausal symptoms, while a healthy one will help manage the symptoms.
That glass of alcohol you take at night could be the reason for your intense night sweats, and the yoga routine you do three times a week might be why you are sleeping better at night. This is especially important for people who have chemopause because their symptoms can be severe.
If you are having severe symptoms, talk to your healthcare provider so they can make recommendations or suggest a therapy plan for you. I found that yoga and a healthy diet were all it took for me to sleep better at night.
Menopause Can Prevent Recurrence Of Cancer
Menopause might be a good thing for people with cancer even before they start treatment. We have established that ovarian hormones increase our risk of cancer. It also means we are more at risk of having a relapse.
However, if menopause is induced before treatment, the risk is negated. Depending on your risk levels, your doctor might suggest medications that will shut down the ovaries or surgical removal.
Other Cancer Treatment Options Can Induce Menopause
Chemotherapy isn’t the only treatment option that induces menopause. While it is the treatment of choice for most cancer conditions, other treatment options can induce early-onset menopause. Any treatment option that stops the production of hormones by the ovaries can lead to menopausal symptoms.
In cancer cases where the ovaries must be removed, menopause becomes total and permanent. In these cases, the symptoms tend to be severe.
Menopause During And After Cancer Treatment Has Its Disadvantages
Menopause might indeed prevent cancer’s chances of returning, but it isn’t as simple as that. Menopause also puts us at risk of several health conditions, including osteoporosis and cardiovascular conditions. Look at it as give and take. Your risk of getting these conditions increases, but in exchange, you are more likely to make a full recovery.
You can also take measures to control and prevent these conditions. Most women would rather bear the discomfort or treatment-induced menopause than risk getting cancer again.
Menopause Doesn’t Cause Cancer But Treating Your Symptoms Can
Menopause does not cause cancer. While it is more likely for women going through menopause to have cancer, it has nothing to do with the condition.
However, during menopause, increased exposure to hormones might increase your chances of getting cancer. Unfortunately, hormone replacement therapy is one of the main treatment methods for menopausal symptoms. Studies have shown that exposure to these hormones might contribute to cancer risk.
To prevent this, talk to your healthcare provider and see what your chances are and the alternative open to you.
Conclusion
As you can see, menopause does not cause cancer; in some cases, it might even be helpful for complete healing.
However, chemotherapy and menopause have a weird connection. Chemotherapy can induce an early form of menopause known as chemo-induced menopause or chemopause. People with this condition present with symptoms of menopause because chemotherapy affects the ovaries and reduces the production of the hormones necessary for menstruation.
Other cancer treatment options also have the capability to induce menopausal symptoms, so ensure you are probably advised before making any decision.