It is no news that many changes occur in women as they enter menopause and go through the postmenopausal experience. We have discussed a handful of these changes and experiences like mood swings, osteoporosis, hot flashes, depression, etc. Still, we are yet to discuss vulvovaginal atrophy and what it entails.
The menopause phase is a university on its own. So, I encourage you to learn as much as possible about it. It will help you understand your changing body and how to respond to the changes. Not just how to respond to the changes but also to understand why these changes occur in the first place. Suppose you have been following this website for a while. In that case, you will already know that low estrogen levels cause most changes during and after menopause, but you are about to know more in this piece.
What Is Vulvovaginal Atrophy
VVA is an acronym for vulvovaginal atrophy. It is one of the postmenopausal symptoms that borders on vagina health issues, it is sometimes called postmenopausal atrophic vaginitis. As a woman, when you go through menopause into postmenopausal experience, please be reminded that part of the things that will change about you is your vagina. This reality is not to scare you if you are not there yet, but you understand it is a normal thing if you are there.
vulvovaginal atrophy can be described as drying both the vulva and vagina skins. It also comes with the thinning of both vulva and vagina skin. vulvovaginal atrophy is one of the things you will notice, and you may not feel comfortable with it because it will affect your sexual interaction with your husband. However, that should not border you much following our previous discussion in that line. There are things you can do, but that’s not our focus here.
vulvovaginal atrophy is a common concern among women. About twenty to thirty percent of women who may have passed the age of forty have this vulvovaginal atrophy. If you are not having vulvovaginal atrophy now, you may exercise patience. However, every woman wants, especially if you enter your postmenopausal phase as a woman.
Cause Of Vulvovaginal Atrophy
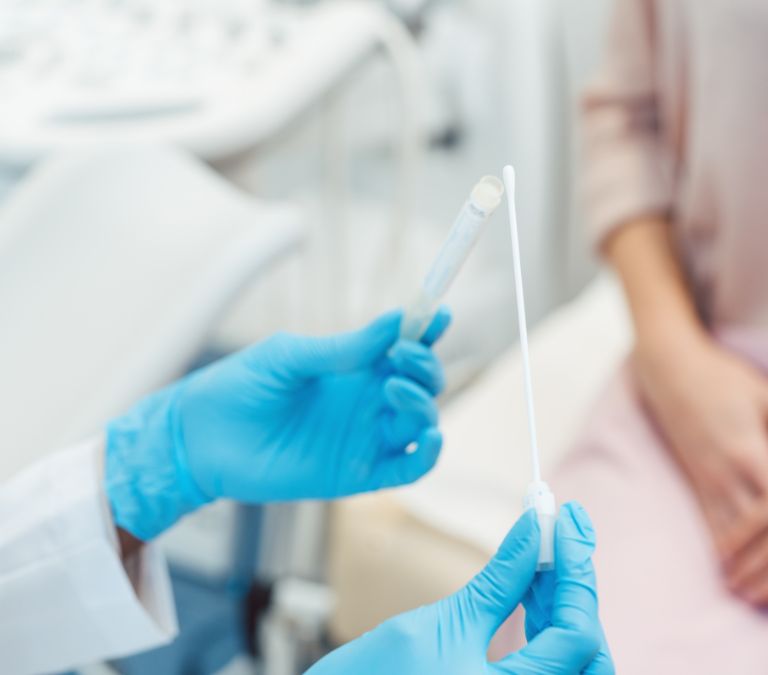
In simple truth, the cause of vulvovaginal atrophy is nothing more than the low level of a hormone called estrogen. As you already know, this hormone does a lot of wonders in women. Still, at menopause, it begins to lower in quantity leading to what is medically known as postmenopausal atrophic vaginitis. Therefore, based on the impact of the low level of estrogen and its impact on menopause, we can say that menopause is the low level of estrogen and its impact.
Normally, estrogen is responsible for a few things that keep the vagina healthy. For instance, it is responsible for ensuring the lubrication of the vagina and also enhancing blood flow to the vagina. With this, the vagina’s health is secured, but as estrogen lowers, the blood flow to the vagina and its lubrication. So, the cause of postmenopausal atrophic vaginitis is the reduction in estrogen levels.
Impact of vulvovaginal atrophy/Postmenopausal Atrophic Vaginitis
Although menopause and postmenopausal symptoms are life impactful generally, after menopause, no woman is the same. The changes are both internal and external. All this information prepares your mind to accept the change and still maximize your life despite the changes.
One such effect of postmenopause experience that causes the change is vulvovaginal atrophy. The impact of vulvovaginal atrophy is not something people notice by sighting the woman; it is felt by the woman alone. The impact is on vagina health and all activities surrounding it.
By activities that surround it, we mean sexual intercourse. Sexual relation with one’s partner indicates where it connects more than a single person. The impact of this is that sex is never the same again. With vulvovaginal atrophy, sex may be painful and uninteresting for both the woman and the partner. It is one of the impacts that affect the relationship of the woman.
Before uninteresting sexual intercourse, it is not out of place for women with vulvovaginal atrophy to experience uncomfortable feelings in the vagina area. This experience is usually the beginning of the vulvovaginal atrophy impacts following postmenopausal experience on the vagina and in a woman.
Vulvovaginal atrophy may negatively impact the urinary system, causing distressing urinary symptoms. Medical practitioners call this genitourinary syndrome of menopause. You will notice that it now covers the health of the vagina as a whole. You have to handle this with great concern as soon as possible.
Symptoms of vulvovaginal atrophy
Some symptoms come with vulvovaginal atrophy; with it, you can easily know if you are having VVA or not. The truth is that many women have vulvovaginal atrophy as postmenopausal experiences. Let’s take a look at a few vulvovaginal atrophy symptoms;
Lack of vaginal lubrication
Lack of vagina lubrication is the initial symptom of vulvovaginal atrophy. It results from the low level of estrogen, which is the major postmenopausal effect. It means that the normal vagina lubricates, ensuring that it is wet. Lubrication is one of the things that ensure the wellness of the vagina.
This lack of lubrication makes sexual intercourse take a new unfavorable turn for the woman and her partner. In addition, it will make penetration difficult because of the friction encountered during sex when vulvovaginal atrophy is still on.
Persistent vaginal dryness
Postmenopause’s consistently low estrogen level causes persistent vagina dryness as vulvovaginal atrophy hits. The problem is really about the persistence in the dryness. As a woman, we experience vagina dryness once in a while before menopause. It sometimes comes during breastfeeding.
With vagina dryness comes pain when exercising, standing, urinating, sitting, etc. I understand how it feels living with the pain from vagina dryness. You can ease off the pain. We shall discuss this in detail later in this piece.
Dyspareunia
Dyspareunia is the medical term used to mean painful sex. As we explain earlier while discussing the lack of vagina lubrication, one of the reasons for this is the lack of vagina lubrication after menopause.
Other factors cause dyspareunia—for instance, breastfeeding, little arousal for sexual intercourse, medications, etc. But the one we are discussing here is the one that originates from postmenopause through vulvovaginal atrophy.
Severe itching
Another symptom of vulvovaginal atrophy is vagina itching. However, vagina itching is not always considered a serious issue. But it may be a pointer to a serious issue sometimes. For instance, it can be a pointer to vulvar cancer, but that is in rare cases. Other causes of severe vagina itching can be a yeast infection, stress, etc.
Severe vagina itching resulting from vulvovaginal atrophy results from the thinning of the vagina wall and possible vagina infection. The dryness of the vagina is also a contributing factor to the itching and may deteriorate the vagina’s health. For this reason, itching must be taken seriously, especially after menopause.
Soreness
Vagina soreness is another symptom of vulvovaginal atrophy. It may come from vagina dryness due to low lubrication during sex. Usually, vagina lubrication enables smooth penetration during sex by taking friction away.
With vagina dryness and low lubrication, sexual intercourse involves a lot of friction. This friction may cause little vagina tears leading to vagina sores. It can also come from little arousal before sexual intercourse. So the first explanation is about vulvovaginal atrophy.
Stinging pain in the vaginal and vulvar area
Stinging pain in the vaginal and vulvar areas is part of the symptoms of vulvovaginal atrophy. It is also linked to the low level of estrogen with postmenopausal experience. It is a pain at the opening of the vagina, which can last as far as you leave it unattended.
This pain can come during vagina bleeding and sex. It may be due to an infection that may result from soreness and vagina dryness. It can make sitting and sex very difficult. If you are already experiencing this in your postmenopausal experience, you should ask your medical practitioner for assistance.
If you carefully read through the vulvovaginal atrophy symptoms, you will discover that all of the symptoms are somehow interrelated. Each of them has a way it links to the other. It would help if you did not embark on self-medication to treat these symptoms. While we appreciate your effort to read through this piece to understand the phase of your life, it is better to handle it properly.
Why Women Don’t Report vulvovaginal atrophy
Over the years, the advice has always been that women should work with their medical doctor through their life’s menopause and postmenopause phases. While menopause and postmenopausal experience are part of a woman’s life, how you respond to it matters a lot.
It is good that you are getting more information about the postmenopausal experience. I appreciate that. It will help you understand your feelings and why you go through those experiences. You must discuss your experience with your medical doctor too. It will help them to provide the best solution each time.
Unfortunately, many women who speak about their menopausal experience with their doctor do not discuss everything with their doctor. I do hope you are not making the same mistake too. Be free to share all your concerns with your medical doctor. Remember that the medical doctor is looking out for your interest to help you maximize this phase of your life.
One common area not usually shared with medical doctors is the vulvovaginal atrophy symptoms. Women have discussed other things like urinary urgency, hot flashes, and vaginal discharge. It has been observed that women do not talk about their experiences, such as dyspareunia, soreness, vaginal itching, etc., which fall under vulvovaginal atrophy symptoms.
Since women don’t discuss vulvovaginal atrophy symptoms they experience, they don’t share with their doctors that they are self-treating these symptoms. Self-medication is one of the things to avoid. You should try as much as possible to avoid that. Only use a treatment path your medical doctor has confirmed is good for you.
Benefits Of Reporting vulvovaginal atrophy
As I mentioned earlier, it is twice important for you to discuss your vulvovaginal atrophy symptoms with your medical doctor. I understand it feels like discussing these symptoms with your doctor, but don’t let pride or shyness stop you from reporting them. You may be saving your pride but dying in silence.
If you don’t report it, then it means that you will be treating them with self-medication. It is not good at all. It will negate the first benefit of discussing these symptoms with your medical doctor. Your medical doctor will give you the best solution. It won’t be the trial and error you will try when you attempt to treat it yourself.
Also, we understand that some women have underlying medical conditions before they enter into menopause or as they go into the postmenopausal experience. It means that medications such a woman can use will be limited to not trigger the underlying medical condition. So, if you have an underlying medical condition, take your health seriously by discussing all with your medical doctor.
Also, another benefit of reporting the symptoms of vulvovaginal atrophy to your medical doctor is that it can help you discover other related health concerns. Some symptoms may seem attributed to vulvovaginal atrophy, but they may point to other serious medical concerns. It is only with the help of a medical practitioner that you will be able to discover this and do the necessary things to help you.
Lastly, discussing all the symptoms of vulvovaginal atrophy will help you get the best medical advice for your everyday living that can help you suppress these symptoms and achieve a healthier lifestyle. Sometimes, this is all you need to improve your life and bid farewell to pains or possibly greater pains.
Hormone Therapies on vulvovaginal atrophy

It is no news that vulvovaginal atrophy is caused by low estrogen, an important hormone in a woman’s system. Since the vulvovaginal atrophy symptoms came as a result of a lack of this hormone, it, therefore, means that making this hormone available in the body will solve the problem with the symptoms.
Your discussion with your medical practitioner will determine whether you will do hormone therapy. There are other ways to treat these postmenopausal symptoms. We have discussed some of these other ways before now. If those ways are best for you, your doctor will let you know based on the level of what is to be treated and your medical history.
After ascertaining that you will be taking estrogen therapy, the next point of action will be to determine how this will be administered. There are a few ways to administer estrogen therapy, depending on what your doctor feels is best for you. That decision depends on your information about your vulvovaginal atrophy symptoms experience, medical history, and personal preference.
This vaginal estrogen therapy can be done either by your doctor’s guide or through the directions you read on each method. There are four methods of estrogen therapy that are good and distinct in their operation. The one you use depends on your unique experience and medical history. Your medical doctor will help you to make a good choice.
Vaginal Estrogen Therapy
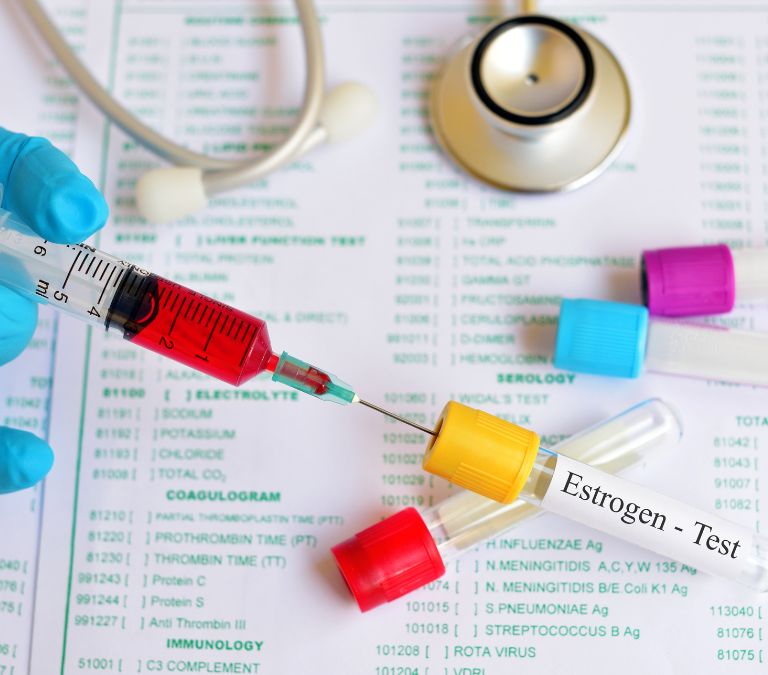
Vaginal estrogen therapy treats low estrogen levels, including application through the vagina. For this type of estrogen treatment, everything is administered through the vagina. The estrogen application through the vagina may come in different forms as we have different ways under this category. Let’s have a short description of how these vaginal estrogen therapy types work below;
Vaginal Estrogen Ring
To use an estrogen ring for vaginal estrogen therapy, here is a description of how to go about it. First, ensure you wash your hands before you begin the process. Then, carefully remove the ring from its pouch. To administer the ring, you may stand, squat, or lie, depending on which is convenient for you. Then hold the ring with the thumb and index finger while you press the sides of the ring together.
Hold your vagina with your other hand while you fold the vagina ring in a figure-eight shape. Place the tip of the ring in the vagina while you push it down carefully. There is nothing to fear because it can’t go beyond your cervix. You may push it more if you don’t feel comfortable with it. There is no rule as to how you have to place it. Just follow these steps to make it comfortable for you.
It is meant to stay three months. Please note that wash it with warm water if the ring falls out before inserting it back. To avoid it from falling out, insert it deeper into your vagina. And if it is lost, replace it with another one, make sure it is up to three months. You can also read the directions or ask your medical doctor how to do it.
Vaginal Estrogen Insert
If you have agreed with your medical doctor to go this way for your vaginal estrogen therapy, here are the steps you need to follow. Begin by washing your hands and making them clean. Make sure your hands are dry before you handle the vaginal insert. Next, insert the vagina insert via the foil of its blister package. Make sure you use your best position to insert it well, whether standing or lying down. Finally, insert it up to two inches deep into the vagina with your finger.
Vaginal Estrogen Tablet
To use the vagina tablet for vaginal estrogen therapy, you will use the applicator, which normally comes with the package. Choose a favorable position to insert the applicator. Carefully place the applicator in your vagina and use the plunger to pull it into your vagina from the applicator. If the tablet falls while trying to insert the applicator, dispose of that tablet. Use another tablet. It is important for your safety. The applicator should not go beyond half of its length into your vagina.
Vaginal Estrogen Cream
It is not a difficult process if you want to use vagina estrogen cream for vaginal estrogen therapy. What is different here is using an applicator that comes with the package. Begin by making sure that your hands are clean. Next, unscrew the cap open and gently press the cream out. Input it into the applicator. Then you place the applicator into your vagina and carefully release the cream into the vagina. You may clean the applicator with warm water and mild soap.
Apart from the above-discussed ways of treating vagina estrogen therapy, another option is hormone replacement therapy. This particular process is not always advisable because of the possible aftermath. However, if you use this process, your medical doctor would have checked the possible advantages against the benefits that will come for you. Therefore, he will advise you accordingly.
Research has shown that possible disadvantages include stroke, breast cancer, heart diseases, blood clots, etc. I am sure you won’t want to bag any of these as you treat postmenopausal symptoms. So, make sure you work with your medical doctor to get the best of your postmenopausal treatments.
The use of hormone replacement therapy is also based on your medical history, age, and whether or not it is only estrogen that will be given or it will be in addition to another hormone. The decision still lies in your doctor’s view; who will know what is best for your health.







