Menopause is the period of every woman’s life where her ovaries lose the ability to produce eggs. To the outside world, this phase kick-starts the phase of a woman’s life where she becomes unable to bear children. However, menopause goes beyond just the loss of periods. Menopause can come with daring and sometimes excruciating challenges in the form of symptoms.
While many women in the United States see the period of menopause as a gateway to freedom from the stress of the reproductive ages, others dread it so much. They wish it never came. Of the women who dread this natural transition, diabetic women go through even more complications during menopause this is because diabetes and menopause are a very tasking combo. With this, one may wonder why diabetic women tend to show more damning menopausal symptoms and how diabetes could make the lifestyle of menopausal women very difficult.
When a woman’s period ceases for 12 consecutive months, menopause is automatically reached. This period of irregular and fluctuating periods is known as perimenopause. While menopause typically begins at the 12th consecutive month of zero periods, the period of perimenopause could last several years and show menopausal symptoms, even when not yet in menopause.
Although perimenopause can start as early as 30, it generally begins between 45 and 55. Women not even in their mid-ages yet could begin to show menopausal symptoms. These symptoms include the characteristic hot flashes, vaginal dryness, moodiness, and even weight gain. These symptoms make the whole menopausal transition quite uncomfortable and complicated. However, weight gain is attributed to even more health complications, including diabetes. Yes, diabetes.
Linking Menopause with Diabetes

Menopause and diabetes are two very different entities; while diabetes is a disease, menopause is a natural transition. However, they both tend to complicate one another.
Diabetes, especially diabetes mellitus, refers to high sugar levels in the blood (hyperglycemia). A decrease or ineffective hormone insulin could cause this increase in blood sugar level. While insulin regulates blood sugar levels, resistance by the body to the insulin hormone will increase the amount of glucose in the blood. So the question is; what could cause insulin resistance in the body? A drop in estrogen and weight gain is the leading cause of insulin resistance.
Effects of Estrogen on Insulin
During menopause, some hormonal changes occur. Hormones responsible for regulating vital metabolic processes in the body tend to go through alarming changes, leading to dangerous health crises. Insulin, the hormone responsible for regulating blood sugar, can go through persistent fluctuations, affecting the glucose level in the blood.
It is essential to know that women at the perimenopause stage of their lives are less at risk of diabetes. However, the risk increases rapidly after crossing menopause. During postmenopause, the estrogen levels in the body begin to go through a steady decline.
While insulin is in charge of regulating blood sugar, estrogen is to optimize insulin. With this, a decrease in estrogen levels in the body will decrease the optimizing power of insulin. At this point, insulin resistance steps in, and the body cannot respond to the insulin hormone as before. With this, the blood sugar increases, and diabetes becomes imminent.
Effects of Weight Gain on Insulin

When glucose levels in the body begin to fluctuate during midlife, such fluctuations could be caused by menopause. Menopausal women are very susceptible to weight gain. As a result of the changes in hormonal levels in the body, menopausal women are likely to experience weight gain.
During menopause, fats no longer move to the hips and buttocks (subcutaneous fat); instead, they accumulate in the abdominal region (visceral fat). Visceral fats can secrete retinol-binding protein, known to cause insulin resistance. The higher the number of abdominal fats, the higher the secretion of retinol-binding protein, and the higher the risk of diabetes.
Could Menopause Be Mistaken for Diabetes?
Due to the striking similarity of menopausal symptoms to diabetes, doctors can give a wrong diagnosis of menopause and mistake it for diabetes. Some symptoms include changes in blood sugar levels, sleeping problems, weight gain, infections, and sexual problems. With this, menopausal women can be mistaken for diabetic patients.
Understanding the Symptoms of Diabetes Mellitus
There are two types of diabetes; type 1 and type 2 diabetes. While type 1 can affect individuals irrespective of age, type 2 only affects individuals during childhood or adolescence. Type 2 diabetes is, however, more common for people in their mid-ages.
The importance of glucose cannot be overemphasized; it serves as fuel for the brain, is an essential source of energy for the body, and is a constituent of the tissues and muscles. However, too much glucose in the body could lead to severe health problems.
The severity of diabetes symptoms varies with the amount of sugar in the blood. It means that more sugar will lead to more severe symptoms. In seriousness, symptoms associated with diabetes include; increased hunger, irritability, frequent urination, extreme thirst, fatigue, blurred vision, slow-healing sores, and frequent infections.
In the United States, about 15 million women have diabetes. It means that 1 in every nine adult women has diabetes. In the United Kingdom, women account for about 44% of adults with diabetes. The persistent occurrence of diabetes among women can be strongly linked to menopause because excess visceral fat has been a leading cause of diabetes.
Understanding the Symptoms of Menopause
Menopause occurs in three stages; perimenopause, menopause, and postmenopause. Perimenopause is the period before menopause. It transitions you into menopause. Postmenopause is the period after menopause. After going through the transition from perimenopause into menopause, post-menopause is automatically reached.
Menopause has symptoms like hot flashes, anxiety, night sweats, and weight gain. Other high severity symptoms include PCOS, ovarian cancer, type 2 diabetes, heart and cardiovascular diseases, endometriosis, and toxic shock syndrome. About 90% of menopausal women will experience more common symptoms like hot flashes and night sweats, while about 20% of menopausal women will experience being diagnosed with diabetes.
How Menopause Increases your Risk of Diabetes
Menopause comes with a variety of complications. Some of these complications can trigger the diagnosis of diabetes. With menopause comes changes in sleeping patterns. Menopausal women tend to experience some decrease in the average amount of sleep they get weekly. Sleep distortion could be caused by the characteristic hot flashes and night sweats during menopause. As a result of these sleeping discomforts, many menopausal women find it very difficult to get long, restful sleep.
This distortion in sleeping patterns makes the body produce cortisol. Cortisol is a hormone responsible for providing the body with enough glucose by utilizing the protein stores in the liver through gluconeogenesis. While cortisol is usually beneficial for the body, long-term secretion of this hormone will lead to an overproduction of glucose, which causes an increase in blood sugar levels. The high amount of cortisol in the body will also cause weight gain in regions less needed by the body; the abdomen. The concentration of fats in the abdominal area can lead to diabetes, triggering a chain reaction of other severe symptoms.
Estrogen, a primary sex hormone in females, is essential for developing physical sex characteristics, maintaining bone health, regulating the menstrual cycle, and regulating cholesterol levels. The importance of estrogen cannot be overemphasized. During menopause, the estrogen levels in the body go through an alarming decline, and this dip could lead to an increase in body fat and abdominal fat. This decline in estrogen levels has not been proven to cause weight gain directly but can be attributed to it. This rapid weight gain during middle age could lead to type 2 diabetes and heart diseases.
Generally, up to 90% of diabetic women are obese. This rapid weight gain causes an increase in the levels of fatty acids in the body. This persistent rise in the fatty acid content of the body will lead to insulin resistance. Insulin resistance is a leading cause of diabetes.
Living with Diabetes while in Menopause
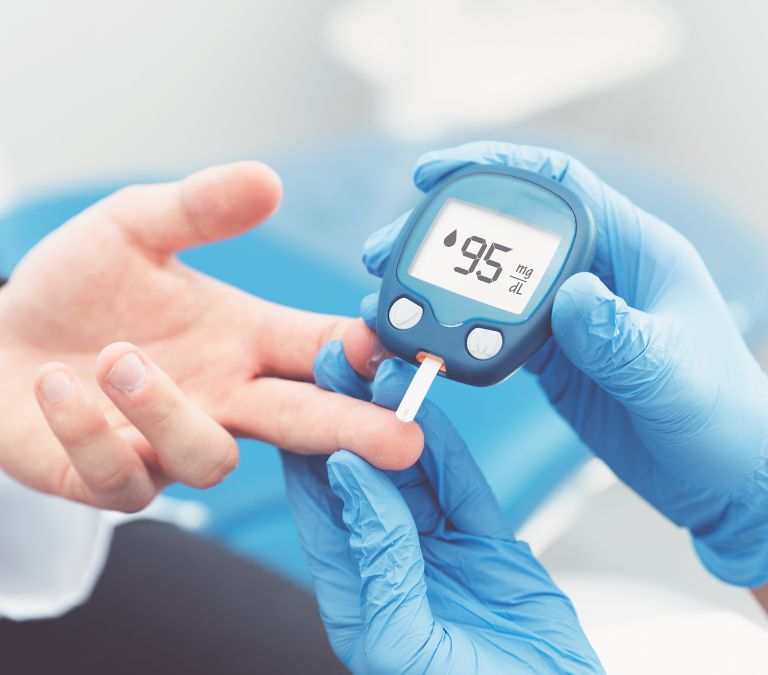
Menopause can make diabetes worse and vice versa. A menopausal woman living with diabetes tends to be at significant risk of severe health complications. While the effect of menopause is different from one woman to another, some common symptoms have been observed among most menopausal women. These symptoms include hot flashes and night sweats. However, symptoms like sleep problems, sexual dysfunction, infections, weight gain, and fluctuating blood sugar levels could also be observed. All of these symptoms make managing diabetes during menopause even more difficult.
Why Staying Together is Lethal: The Tale of Two Friends – Menopause and Diabetes
Menopause comes with its problems, so as diabetes. Menopause, although natural, can trigger the occurrence of some severe symptoms. Diabetes, on the other hand, is a disease caused by high amounts of glucose in the blood. These two are very different entities.
However, a menopausal woman living with diabetes is more susceptible to more symptoms of even higher severity. With this, managing diabetes becomes very difficult. Answering how menopause increases the risk of diabetes hasn’t been very easy for researchers to answer. The effects of menopause are usually seen as effects that come with aging and weight gain.
However, age and being overweight are the two most common factors influencing diabetes. It means menopause can have an indirect effect, knowing that it causes weight gain and is a phase of life that comes with age. When diabetes and menopause happen concurrently, they can cause awful complications like:
Fluctuating Blood Sugar Levels
The fluctuating blood sugar levels of a menopausal woman cause sudden changes in the estrogen and progestogen levels of the body. These changes decrease the body’s sensitivity to the insulin hormone. It can lead to insulin resistance and could make managing diabetes and menopause very tasking.
Managing diabetes means trying to balance the sugar levels in the body. If the body still produces so much glucose caused by altering the optimizing power of insulin in the body, the blood sugar will continue to go through persistent fluctuation. Rapid increase and decrease in the blood sugar level will only make menopause and diabetes more difficult to live with.
Rapid Weight Gain
Menopausal women are very likely to experience weight gain. Due to weight gain on blood sugar levels, some adjustments might have to be made in managing diabetes.
Inadequate Sleep
Women going through menopause often complain of inadequate sleep. Hot flashes and night sweat often cause this lack of good sleep. While insufficient sleep is often regarded as no big deal, it is essential to know that not having enough sleep will cause weight gain. Yes, weight gain. And we all know how weight gain could cause diabetes.
If menopause makes you sleep-deprived, being diabetic at that same time will make management options less effective. Menopausal women living with diabetes are likely to show more severe menopausal symptoms. High blood sugar comes with symptoms like rapid heartbeat, vomiting, vision problems, excessive hunger and thirst, and nerve problems. When linked with the symptoms of menopause, it becomes life-threatening and challenging to manage.
In a nutshell, managing diabetes during menopause is very difficult.
Dealing with the Twin Problems of Diabetes and Menopause
The good news about this problem is that you can manage it effectively. Yes, even during menopause, you can still adequately address diabetes. Having diabetes during menopause isn’t a death sentence and shouldn’t be taken as one. It is known that menopause can increase the impact of diabetes on you. Improving menopause management patterns will help reduce its impact on your diabetes control process and general health. Managing diabetes during menopause becomes more effective with the best management options.
I Have both Diabetes and Menopause – How Do I Go about It?
For managing diabetes and menopause, the best option remains lifestyle changes. However, various options have proven effective enough to get the best results.
Lifestyle Changes
Menopause is a natural part of life and shouldn’t be considered an illness. All women must go through menopause. With every phase of life comes changes. To manage diabetes during menopause, you must be ready to adapt to changes to live healthier, happier, and longer lives. You can adopt certain lifestyle changes to manage diabetes and menopause. Some of the lifestyle changes are discussed below.
Exercising Regularly

Engaging in regular exercises can be a stimulant for improved metabolism and fitness, decreased stress, and better sleep. Research shows that living a healthy lifestyle is the best way to manage diabetes. In another study, engaging in routine exercise will decrease some diabetic effects on you by up to 31%.
I love biking, and sometimes, I ride my bike for long distances on weekends. Go swimming, hop on the treadmill and get those legs busy. For a start, why not stand on one foot while brushing your teeth? Or doing ten squats before entering the bathtub?
Not only does regular exercise help to keep fit, but it also helps the mind to stay healthy. All of these are effective ways of managing diabetes and menopause. Exercises help improve not only your physical health but also your mental health. It means you can alleviate menopausal and diabetic symptoms like fatigue, anxiety, obesity, and poor sleep through exercise.
Maintaining a Healthy Weight
Excess body fat around the waist increases the risk of developing diabetes and heart diseases. Also, according to studies, losing up to ten pounds of weight within a year can help eliminate vasomotor symptoms like night sweats and hot flashes. Maintaining or aiming for a healthy weight when diagnosed with diabetes is essential.
Burning visceral fats will be an excellent way to start. Maintaining a healthy weight should be prioritized if you are going through menopause and diabetes. No matter how small, try some exercises, stretch once or twice every day, jog the length of your street, try yoga, and use the staircase instead of the elevator. It’ll help in the long run. It might not be easy, but it’s effective.
Avoid Skipping Meals
Have a regular pattern of eating and do not skip meals. Besides hindering weight loss efforts, irregular eating patterns can aggravate some menopausal symptoms. Eat healthily and maintain a fixed time frame for every meal eaten. It can be challenging to keep up with a fixed pattern, but if you can abide by it for a few weeks, it becomes easy to follow.
Smile More and Stay Happy
Staying happy can help you relieve stress and boost your immune system. The period of menopause can be challenging, sometimes excruciating. Adding diabetes to the radar will only make matters worse. Nevertheless, always remember that a happy mind is a healthy mind. Try taking up new challenges to keep yourself busy and active.
Find positive social support and talk to other women going through menopause. Find things that make you happy. It might be going to the concert you’ve always dreamed of. It may be buying that dress you’ve always fancied. You may spend quality time with people you love or even listen to a classic Beyoncé album. A happy mind is a healthy mind. Don’t forget that.
Diet Changes

The goal of every diabetic patient is to reduce their blood sugar level. I am not a huge fan of medicine. Sure they can prove helpful, but I always seek other ways to cure an illness before settling for medication.
According to research, coffee, whether caffeinated or decaffeinated, can help reduce your risks of getting type 2 diabetes. It is because coffee is known to help improve sugar metabolism in the body. However, coffee also aggravates menopausal symptoms like hot flashes and night sweats.
According to The Food and Drug Administration, caffeine is not harmful, and few people have experienced adverse reactions. However, diabetic women in the postmenopausal phase of their lives must try as much as possible to control the average intake of caffeinated products in their system to prevent worsening vasomotor symptoms. If you take coffee but do not experience severe menopausal symptoms, you can keep taking it solely to manage diabetes.
Also, highly spicy and sugary foods should be limited. If you love your pasta extra spicy, or you want your ice cream extra sweet, I’d say you reduce the amount of spiciness or the amount of sugar you take. It will help if you cut down on alcoholic beverages and cigarettes.
These food products trigger menopausal symptoms and make diabetes difficult to manage. With this, it becomes a wise decision to limit its intake.
So, with all these, some may ask what food should be eaten more by diabetic women going through the postmenopausal phase of life. As usual, fruits and vegetables are the preferred foods for diabetic patients. Not only do they help to ease the problems of diabetes, but they also help cushion the symptoms of menopause and live a healthier life.
Some foods to embrace as a diabetic patient during menopause include fruits and veggies like spinach, kale, and collard greens, and foods rich in Calcium and vitamin D like milk, cheese, yogurt, tofu, sardines, beans, cereals, fish, eggs, and cod liver oil, foods rich in phytoestrogens like flaxseeds, soybeans, sesame seeds, tempeh, and linseed, protein-rich foods like meat, nuts, and legumes. Less sugar, more veggies. Remember this formula. Drink lots of water.
Controlling blood sugar is essential not just for menopausal women but for humans. It is vital to go for regular tests to check your blood sugar. A large percentage of menopausal women live with diabetes without knowing about it. Your health should be taken seriously, and having an accessible doctor feels very suitable.







