Article Insights & Reflections
Synopsis: This overview brings clarity to a key menopause topic and translates research into practical next steps. It equips readers with options to discuss with a qualified clinician and tools to start improving today.
Top 5 Questions Answered:
- Which symptoms are truly driven by menopause?
- What options exist beyond over-the-counter fixes?
- When should I consider medical therapy?
- Which daily habits make the biggest difference?
- How do I personalize a plan that lasts?
Menopause is reached when a woman’s body stops producing the reproductive hormones that cause the monthly menstrual flow. A woman is said to have reached menopause when she spends 12 months in a row without seeing her menstrual cycle.
This natural transition happens in three 3 stages:
 One of the best ways to decrease your risk of heart disease is to quit tobacco. Statistics have shown that about 21% of American women 18 years or older smoke. If you’re among them, it’s time to eliminate cigarettes. Excess tobacco leads to plaque in blood vessels, which reduces good cholesterol, elevates blood pressure, and causes heart arrhythmia. Research has shown that women who smoke have five times more chances of developing heart conditions than women who don’t smoke.
One of the best ways to decrease your risk of heart disease is to quit tobacco. Statistics have shown that about 21% of American women 18 years or older smoke. If you’re among them, it’s time to eliminate cigarettes. Excess tobacco leads to plaque in blood vessels, which reduces good cholesterol, elevates blood pressure, and causes heart arrhythmia. Research has shown that women who smoke have five times more chances of developing heart conditions than women who don’t smoke.
 A high number of women experience depression during perimenopause. Research has shown that menopausal transitions, especially perimenopause increases the risk of depression among women due to fluctuations in hormone levels.
Hormone changes aren’t the only cause of depression during menopause. Psychological factors and issues like the loss of a partner, excessive consumption of alcohol, health conditions, and physical disability also play a role.
Generally, women under chronic stress, experiencing major life events, or having underlying medical conditions are at higher risk of being depressed at perimenopause.
However, evaluating menopause depression can be challenging because many hormonal fluctuations symptoms experienced by menopausal women are similar to symptoms of depression.
Here are signs and symptoms of depression you should always check out for:
A high number of women experience depression during perimenopause. Research has shown that menopausal transitions, especially perimenopause increases the risk of depression among women due to fluctuations in hormone levels.
Hormone changes aren’t the only cause of depression during menopause. Psychological factors and issues like the loss of a partner, excessive consumption of alcohol, health conditions, and physical disability also play a role.
Generally, women under chronic stress, experiencing major life events, or having underlying medical conditions are at higher risk of being depressed at perimenopause.
However, evaluating menopause depression can be challenging because many hormonal fluctuations symptoms experienced by menopausal women are similar to symptoms of depression.
Here are signs and symptoms of depression you should always check out for:
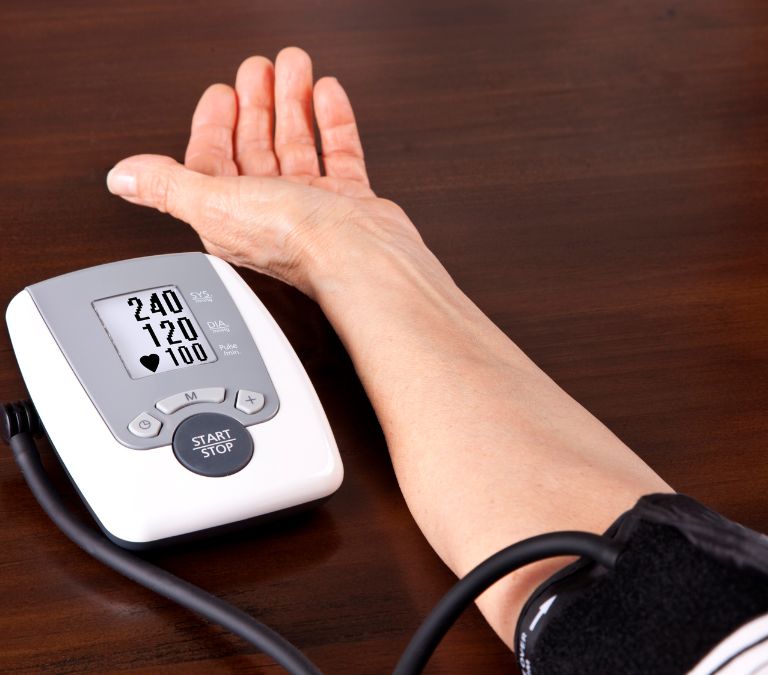 While many believe that men are affected more by high blood pressure, the American Heart Association has proved that more than 50 percent of high blood pressure death victims are women.
Women experience high blood pressure as they reach menopause. Studies have shown that high blood pressure is prevalent in all three stages of menopause.
A recent study in 2020 has shown that early menopause also increases the risk of high blood pressure.
The changes in blood pressure during menopause are due to a drop in estrogen levels. The hormone has been linked with vasodilatory effects that help keep the blood vessels wide enough to support proper blood flow and maintain lower blood pressure.
Also, weight gain during menopause increases women’s risk of high blood pressure.
In most cases, symptoms of hypertension are only experienced when the condition has worsened. Some of the symptoms include:
While many believe that men are affected more by high blood pressure, the American Heart Association has proved that more than 50 percent of high blood pressure death victims are women.
Women experience high blood pressure as they reach menopause. Studies have shown that high blood pressure is prevalent in all three stages of menopause.
A recent study in 2020 has shown that early menopause also increases the risk of high blood pressure.
The changes in blood pressure during menopause are due to a drop in estrogen levels. The hormone has been linked with vasodilatory effects that help keep the blood vessels wide enough to support proper blood flow and maintain lower blood pressure.
Also, weight gain during menopause increases women’s risk of high blood pressure.
In most cases, symptoms of hypertension are only experienced when the condition has worsened. Some of the symptoms include:
-
Perimenopause is the stage is leading to menopause. At this phase, the production of reproductive hormones declined, and the monthly cycle became irregular. Also, women start to experience the side effects of menopause.
-
Menopause: is when the production of reproductive hormones has stopped, and the monthly period has stopped. This marks an end to the reproductive years of a woman. Immediately after this stage, a woman is said to have entered postmenopause.
-
Postmenopause is the stage after the menstrual cycle has stopped. Postmenopause lasts till the end of your life – the hormone levels will be very low, and you won’t experience menstruation again. Also, you can’t conceive because the ovaries no longer release eggs.
1. Heart Disease:
At some point, we all thought heart disease is a man’s condition. But nay! Heart disease is among women’s most common causes of death. Research has shown that cardiovascular conditions are the cause of more than half of the deaths of women over the age of 50. The risks of cardiovascular diseases increase for everyone as they age; however, the rate at which the risk of heart disease increases in women over 50 is very high. Also, studies have shown that young women that have undergone surgical menopause and didn’t undergo Hormone Replacement Therapy are more likely to develop heart conditions. However, you must know menopause is a natural process that doesn’t cause heart diseases. However, risk factors increase during menopause, and some unhealthy lifestyles in early life can also have an effect. Menopause women who have these lifestyle practices or health conditions are more likely to develop heart conditions:- Smoking
- Overweight
- High level of LDL (Bad cholesterol)
- Low levels of HDL (Good Cholesterol)
- Sedentary Lifestyle
- High blood pressure
- Diabetes
- Family history of cardiovascular disease
Does Estrogen Play a Role?
Well, menopause is all about estrogen, estrogen, and estrogen. But does it have a role to play in cardiovascular conditions? Research has shown that estrogen helps keep the blood vessel’s inner lining flexible. During menopause, the levels of estrogen decline; thus, the blood vessels become affected. Since there’s less estrogen, it becomes easier for cholesterol to build up on the walls of the blood vessels. These vessels lead to the heart and brain; as such, too much buildup in them increases the risk of cardiovascular conditions and stroke.Ways to Reduce Risk of Heart Disease At Menopause:
Some factors that expose us to the risk of heart disease are things we cannot control, like family history and aging. But there are still some things you can do to reduce your risks. Below are some:Quit Smoking:
 One of the best ways to decrease your risk of heart disease is to quit tobacco. Statistics have shown that about 21% of American women 18 years or older smoke. If you’re among them, it’s time to eliminate cigarettes. Excess tobacco leads to plaque in blood vessels, which reduces good cholesterol, elevates blood pressure, and causes heart arrhythmia. Research has shown that women who smoke have five times more chances of developing heart conditions than women who don’t smoke.
One of the best ways to decrease your risk of heart disease is to quit tobacco. Statistics have shown that about 21% of American women 18 years or older smoke. If you’re among them, it’s time to eliminate cigarettes. Excess tobacco leads to plaque in blood vessels, which reduces good cholesterol, elevates blood pressure, and causes heart arrhythmia. Research has shown that women who smoke have five times more chances of developing heart conditions than women who don’t smoke.
Be Mindful of Your Blood Pressure:
High blood pressure is a core factor that increases the risk of heart failure, heart attack, heart disease, and other serious health complications. Unfortunately, symptoms of hypertension aren’t usually understood until the damage has been done. So, the best thing to do is to stay alert about your blood pressure. Here’s a tip: the systolic blood pressure shouldn’t be more than 120mmgHg, while the diastolic blood pressure shouldn’t be more than 80mmHg.Exercise Regularly
We all wouldn’t mind spending the whole day on the couch watching soap operas and reading magazines, but that isn’t good for our heart health. Get on the move! Set a weekly workout goal of at least 150 minutes. It doesn’t have to be a rigorous exercise; even a 30-minute walk or jog can do.Maintain a Healthy Weight
Studies have shown that being overweight contributes to the development of heart disease. Here’s why – the more your weight, the harder your heart has to work to ensure a proper supply of nutrients to all body parts.2. Osteoporosis
Osteoporosis is a health condition that causes a decrease in bone mass and strength, thus weakening the bones and making you more prone to fractures. In most cases, osteoporosis doesn’t show any symptoms. Experts are still yet to figure out the exact cause of osteoporosis, but some have linked it to aging. Between the age of 25 to 30, women reach their peak in bone strength and mass. At that age, the skeleton stops growing, and the bones are at their strongest stage. Estrogen greatly impacts the growth of bones and maintaining their strength. During menopause, estrogen levels drop drastically, resulting in bone mass loss. Women with thin bone mass before menopause are more likely to experience bone loss and osteoporosis at menopause. A study has shown that women experience up to 20 percent bone loss at menopause, and at least 1 in every 2 women over 60 is affected by osteoporosis and is likely to suffer a bone fracture. Factors that expose you to osteoporosis include:- Age: After the peak bone mass is reached 30 years, your bone mass starts to decline as you age.
- Gender: Research has shown that females are more likely to develop osteoporosis than males
- Race: Studies have shown that Asian and Caucasian women are more likely to develop osteoporosis and suffer from fractures
- Body weight: Slim women are more likely to develop osteoporosis than fat women.
- Side effects of medications: Long-term use of certain medication like steroids have been linked with higher risks of osteoporosis
- Family History: Heredity has also been linked to an increased risk of osteoporosis.
Ways to Reduce Risk of Osteoporosis During Menopause?
Certain lifestyle changes can greatly reduce your risk of osteoporosis during menopause.Increase Calcium Intake:
Calcium has been linked to the growth of healthy bones. Include calcium-rich foods in your daily diet, like dairy products, tofu, Brazil nuts, salmon, sardines, almonds, and soy. Experts recommend you should intake 1300mg of dietary calcium daily.Don’t Joke with Vitamin D
Another good way to prevent osteoporosis is by maintaining adequate vitamin D. This nutrient makes it easier for your body to absorb calcium. While our body naturally makes vitamin D after exposure to the sun, you can increase your vitamin D levels by taking foods rich in the nutrient.Engage in Physical Activities:
Avoid a sedentary lifestyle. Engage in regular aerobic exercises like running and jogging. Weight-bearing exercises such as weight training and brisk walking are also encouraged. However, it would help if you avoid high-impact activities.Reduce Alcohol and Caffeine Intake:
Menopausal women are advised to reduce alcohol intake to the barest minimum. You should stick to one drink of alcohol daily with at least 2 alcohol-free days weekly. Also, excess caffeine intake should be avoided. Can’t you do without your morning and evening cup of Joe? Replace it with a healthier drink.3. Weight Gain
As you age, maintaining a healthy weight becomes very hard. In most cases, women experience a significant increase in weight during menopause. As we know, menopause is characterized by hormonal fluctuations which affect us in several ways. One of these is excess weight gain around the abdomen. Research has shown that about 30% of women aged between 50 to 59 are obese. This is a sign that menopause and weight gain go hand in hand. Changes in the levels of estrogen influence the distribution of fats in the body; this is why perimenopause and postmenopause women gain more unwanted fat in the abdominal part of the body. Women store fats in the lower parts of the body at young age, making them develop a sexy shape. As they age, more fats are deposited around the abdomen, giving them a round shape. However, hormonal changes aren’t the only cause of weight gain in menopause. Other factors like aging, genetics, and lifestyle choices can cause weight gain during menopause. For example, if you have a family history of obesity or excess abdominal fat, you’re likely to develop it too. Aging also plays a role – muscle mass decreases as you age, leading to a decrease in the rate of metabolism. This makes it hard for you to maintain a healthy weight. It becomes more harder if you eat unhealthy foods and don’t exercise.Ways to Reduce Risk of Weight Gain in Menopause
Weight gain at menopause isn’t inevitable; with some simple lifestyle changes, you’ll be able to maintain a healthy weight:Exercise More:
Moving is one of the best ways to shed excess weight. As you develop muscles, your metabolism becomes more effective, making it easier to maintain a healthy weight.Eat Healthily:
As you age, your body needs fewer calories than it did in your 20s and 30s. However, it would help if you watched nutrition while cutting calories. Load more leafy greens, fruits, legumes, nuts, and whole grains. Avoid processed foods and sugary food. Limit the intake of beef and poultry to the minimum level.Limit Alcohol Intake
Too much consumption of alcohol has been linked to excess calories and an increased risk of being overweight. Cut off alcoholic beverages and replace them with fruit juices and smoothies.4. Low Sex Drive
Many women experience changes in their libido as they go through menopause. Few women experienced increased sex drive while others experienced decreased sex drive. Experts have linked low sex drive during menopause to hormonal fluctuations. Also, women experience symptoms like depression and mood swings during menopause, making them less interested in sex. During menopause, estrogen and testosterone levels drop drastically, making it hard for women to get aroused. Also, vaginal dryness and tightness are experienced because of a fall in estrogen levels. When estrogen is low, the blood supply in the vagina is affected, causing it to be less lubricated. This sometimes leads to thinning of the vaginal wall, which causes pain during sex. Also, some physical changes like weight gain can affect your sexual drive. Many women feel uncomfortable with their bodies, thus leading to decreased libido.Ways to Treat Low Sex Drive During Menopause
There are a lot of ways you can increase your sex drive while going through the menopause transition. Below are some:Hormone Replacement Therapy
One of the best ways to treat low libido during menopause is by increasing your estrogen levels through Hormone replacement therapy. Taking estrogen pills or using patches provides your vagina with the hormones the body no longer makes. However, it would help if you talked to your doctor before starting HRT, as it can expose you to health complications.Vaginal Lubricant
Consider using vaginal lubricants to reduce dryness and make sex less painful. This helps, especially if painful sex due to vaginal dryness is your cause of low sex drive.Focus on Intimacy
There are other ways to feel close to your partner apart from sex. If you’re experiencing low libido, consider caressing, kissing, and other intimate acts with your partner, which can help arouse you.5. Vaginal Atrophy
Atrophic vaginitis is a genitourinary disorder in which the vaginal lining becomes thinner and dryer due to a lack of estrogen. This condition is mostly experienced during menopause when there are fluctuations in hormone levels. However, younger women can also be affected when their estrogen level is not balanced. Studies have shown that about 40 percent of postmenopausal women experience the symptoms of vaginal atrophy. The conditions result in experiencing pain during sex and expose women to urinary tract infections and frequent urination. During menopause, the vaginal wall becomes thinner, and the vaginal canal becomes more narrow due to a lack of estrogen. Also, there will be less secretion of vaginal fluids that naturally lubricate the place. The acid balance of the vagina is also disturbed during menopause. These lead to vaginal atrophy. Symptoms of atrophic vaginitis include:- The vaginal wall becomes thinner
- Compressing the vaginal opening
- Vaginal dryness
- Pain during sex
- Bleeding after sex
- Itchy vulva
- Yellowish discharge
- Pain during urination
- More urinary tract infections
- Involuntary leakage of urine
- Women who haven’t given birth vaginally are more likely to develop the condition than those who have given birth vaginally.
- Lack of intercourse
- Exposure to radiation or chemotherapy
- Loss of placental reproductive hormone
- Excess smoking of tobacco
- Taking medications with anti-estrogen effects
- Surgical removal of ovaries
- Breastfeeding
Ways to Treat Vaginal Atrophy
With the right treatment plan, you can combat vaginal atrophy and improve your vaginal health. Below are some tips;Topical Estrogen:
Topical estrogen involves increasing your estrogen levels through the skin. Balanced hormone levels can help relieve symptoms of vaginal atrophy, such as dryness and thin vaginal wall. Topical estrogens are available in different forms – there are vaginal rings that are inserted into the upper part of the organ. There are vaginal estrogen creams that are placed into the vagina before going to bed. And some tablets are inserted using an applicator. All these forms of topical estrogen release doses of the hormone slowly in your blood, thereby regulating its balance.Wearing Cotton Panties
Using cotton underwear and loose clothes can assist in the proper circulation of air in the vaginal. This makes the environment less ideal for harmful organisms.Stay Sexually Active
Though women suffering from vaginal atrophy experience pain during sex, experts recommend staying sexually active. Sexual intercourse improves blood circulation to the vagina and helps keep it lubricated.Use Lubricants and Moisturizers
Lubricants add moisture to the vagina, prevent dryness, and make sex more comfortable. Moisturizers, on the other hand, help relieve irritation and reduce dryness.6. Urinary Incontinence (UI)
Though urinary incontinence can be experienced at any stage of life, menopause increases the risk of developing the condition. Dropping in estrogen levels during menopause causes the linings of the urethra to thin, and the pelvic muscles become more relaxed and weaker. The lower your estrogen levels, the more you become exposed to urinary incontinence. Urinary incontinence means loss of bladder control, and millions of women experience it as they reach the age of menopause. The condition, however, doesn’t mean you’ve lost total control of your bladder – usually few drops of urine will leak when you laugh or cough, and you might not be able to keep urine before you reach the toilet. Like any other menopause complications, the risk of urinary incontinence can increase due to some factors, including:- Excess Intake of Caffeine or Alcohol: Drinking alcoholic beverages and caffeine fills the bladder quickly, making you urinate more.
- Obesity: Being overweight puts more pressure on your bladder, thus increasing your risk of developing UI
- Medications: Intake of certain medications such as steroids can increase your risk of developing UI
- Never damage: When the nerves are damaged, signals won’t be properly transmitted from the bladder to the brain, so you won’t feel the urge to urinate.
- Chronic constipation weakens the pelvic muscles and makes them less able to control the bladder.
Ways to Treat Urinary Incontinence
The treatment options for urinary incontinence are many and depend on the type of UI you’re experiencing and the cause. However, there are small lifestyle changes that can help;Practice Kegel Exercises
Kegel exercises are physical activities that involve tightening the pelvic muscles for a while then releasing them. There are different Kegel exercises – choose the one that works best for you and practice it regularly.Be Mindful of What You Drink.
Reduce the intake of alcohol, soda beverages, and caffeine. Menopausal women are advised not to drink more than one alcohol per day. Also, reduce your liquid intake in the evenings to prevent waking up several times in the night to pee.Preplan your Visits to the Toilet
Make a bathroom trip schedule – for example, after every 90 minutes. This helps you to retain control over your bladder.7. Depression
 A high number of women experience depression during perimenopause. Research has shown that menopausal transitions, especially perimenopause increases the risk of depression among women due to fluctuations in hormone levels.
Hormone changes aren’t the only cause of depression during menopause. Psychological factors and issues like the loss of a partner, excessive consumption of alcohol, health conditions, and physical disability also play a role.
Generally, women under chronic stress, experiencing major life events, or having underlying medical conditions are at higher risk of being depressed at perimenopause.
However, evaluating menopause depression can be challenging because many hormonal fluctuations symptoms experienced by menopausal women are similar to symptoms of depression.
Here are signs and symptoms of depression you should always check out for:
A high number of women experience depression during perimenopause. Research has shown that menopausal transitions, especially perimenopause increases the risk of depression among women due to fluctuations in hormone levels.
Hormone changes aren’t the only cause of depression during menopause. Psychological factors and issues like the loss of a partner, excessive consumption of alcohol, health conditions, and physical disability also play a role.
Generally, women under chronic stress, experiencing major life events, or having underlying medical conditions are at higher risk of being depressed at perimenopause.
However, evaluating menopause depression can be challenging because many hormonal fluctuations symptoms experienced by menopausal women are similar to symptoms of depression.
Here are signs and symptoms of depression you should always check out for:
- Persistent feelings of moodiness, sadness, anxiety, apathy, and hopelessness.
- Chronic fatigue and lack of energy
- Irritability
- Lost interest in activities you enjoy before
- Insomnia or oversleeping
- Finding it difficult to concentrate or make decisions
- Feeling worthless
- Headaches and digestive problems
- Suicidal thoughts
- A family history of depression
- A personal history of depression
- Premenstrual dysphoric disorder
- Postpartum depression
- Excess stress
- Surgical menopause
- Lifestyle choices
- Underlying medical conditions
Treatment for Menopausal Depression
For menopausal women, certain therapeutic options have been proven to help. These include a combination of psychotherapy with antidepressant medications. There are different types of psychotherapy. However, cognitive behavioral therapy (CBT) has been proven to be one of the best for treating menopausal depression. Also, psychotherapy will help you easily identify the factors contributing to depression, such as excess stress or lifestyle choices. Your therapist can help you overcome these factors easily. Also, there is some evidence that menopause replacement therapy may help reduce mood swings. However, the Food and Drug Administration (FDA) is yet to approve menopause replacement therapy as a treatment for menopausal depression. However, the therapy can help relieve symptoms like hot flashes and insomnia, affecting mood. In some cases, your doctor might recommend Selective Serotonin Reuptake Inhibitors, which alter the levels of neurotransmitters, thereby reducing the symptoms of depression. There are a lot of lifestyle choices that can help you cope with menopausal depression. For example, exercising daily or taking a walk with your pet. Going out with family or friends and participating in activities elevate your mood and make you happy. Quitting smoking, alcohol, and other unhealthy foods can also help in managing symptoms of menopausal depression.8. High Blood Pressure
 While many believe that men are affected more by high blood pressure, the American Heart Association has proved that more than 50 percent of high blood pressure death victims are women.
Women experience high blood pressure as they reach menopause. Studies have shown that high blood pressure is prevalent in all three stages of menopause.
A recent study in 2020 has shown that early menopause also increases the risk of high blood pressure.
The changes in blood pressure during menopause are due to a drop in estrogen levels. The hormone has been linked with vasodilatory effects that help keep the blood vessels wide enough to support proper blood flow and maintain lower blood pressure.
Also, weight gain during menopause increases women’s risk of high blood pressure.
In most cases, symptoms of hypertension are only experienced when the condition has worsened. Some of the symptoms include:
While many believe that men are affected more by high blood pressure, the American Heart Association has proved that more than 50 percent of high blood pressure death victims are women.
Women experience high blood pressure as they reach menopause. Studies have shown that high blood pressure is prevalent in all three stages of menopause.
A recent study in 2020 has shown that early menopause also increases the risk of high blood pressure.
The changes in blood pressure during menopause are due to a drop in estrogen levels. The hormone has been linked with vasodilatory effects that help keep the blood vessels wide enough to support proper blood flow and maintain lower blood pressure.
Also, weight gain during menopause increases women’s risk of high blood pressure.
In most cases, symptoms of hypertension are only experienced when the condition has worsened. Some of the symptoms include:
- Severe headache
- Extreme fatigue
- Palpitations
- Nosebleeds
- Anxiety
- Shortens of breath.
- Lower levels of estrogen lead to a lack of vasodilators
- Obesity
- Excessive consumption of alcohol
- Too much intake of salt
- High levels of bad cholesterol (LDL)
- Unwholesome diet
- Diabetes
- Overweight
- Sedentary lifestyle
- Family history of high blood pressure
- Race or ethnicity
- Smoking and drinking alcohol
Natural Remedies For Controlling High Blood Pressure
Regular Exercise:
Studies have shown that exercising lowers blood pressure by 8 numbers. When you engage in physical activities, your blood pressure remains healthy. Also, moving your body makes the heart stronger and aids the pumping of blood.Minimize Sodium Intake
Most Processed food contains a lot of sodium. Too much intake of sodium exposes you to high blood pressure. Consider reducing your sodium (salt) intake to less than 2300mg daily.Walk Out of Stress
Walking out of stress goes a long way In helping you manage your blood pressure. There are many ways to relieve stress; choose the one that works best for you and practice regularly.Conclusion:
If you are experiencing any of these conditions you should seek out a qualified medical professional for help.
Post Views: 3,365







