Pregnancy and Menopause is 0ne of the most searched terms on search engines. This is because the transition into menopause comes with worries and implications. The process remains confusing for most women, even those experiencing menopause. They wonder about many things and question the normalcy of most of their symptoms. One of the things most of them worry about is if they can ever get pregnant again. In this article, we will be discussing menopause and pregnancy.
There are two groups of women who think about the possibility of them getting pregnant even during or after menopause. First, some do not want to risk giving birth at such a phase in their life, and they would do anything to negate this possibility. Then some want to have kids after menopause because of one reason.
The baseline is that answering this question is important. It would be relevant in making birth control decisions and family planning.
It’s not impossible to get pregnant if you’re experiencing hot flashes, mood swings, and irregular periods which are some of the symptoms of menopause. However, it does mean you’re probably not as fertile as you once were.
You haven’t technically hit menopause until you have gone a whole year without experiencing a period. Once you have reached menopause, your hormone levels have decreased, so your ovaries will no longer release eggs. Therefore, it is presumed that it is no longer possible to conceive naturally.
The changes your body undergoes do not support reproduction. Instead, your body produces the hormones estrogen, progesterone, luteinizing hormone (LH), and follicle-stimulating hormone (FSH) during your reproductive years. LH, FSH, and estrogen function synergistically in the middle of your monthly cycle to cause your ovaries to release a mature egg during ovulation. This egg fertilizes with a sperm cell and leads to possible pregnancy.
To understand the chances of getting pregnant after menopause, one must understand the events leading to menopause. Over the past years, people have considered menopause as the process leading up to that significant event. Therefore, understanding what happens during this transition will help you know the chances of getting pregnant during this phase.
Pregnancy and Menopause

When a woman has not had her period for a whole year without any other underlying causes, she is retrospectively diagnosed with menopause. While menopause is considered a single event, it is not isolated. Other physiological changes lead up to this event. Most people associate symptoms with menopause start happening before the years leading to menopause. This period is termed perimenopause.
Perimenopause usually presents with a fall in the hormone estrogen. This fall will trigger other physiological reactions that bring about the symptoms witnessed during this period. Estrogen is produced by your ovaries and is important for the reproductive system to function properly. As you approach perimenopause, your estrogen levels drop. Progesterone, another hormone generated by the ovaries, becomes imbalanced as estrogen levels fall. These two hormones regulate ovulation and menstruation.
During perimenopause, hormone levels frequently vary. During perimenopause, your body has started the process of bringing an end to its reproductive clock. During perimenopause, the menstrual cycle becomes erratic due to fluctuations in hormone levels. The flow might become inconsistent, and sometimes the cycle might not occur completely, leading to the menstrual flow not occurring.
The issue about perimenopause is that it affects different women in different ways. For some women, perimenopause may begin in the mid-50s, while it may begin as early as the mid-30s. This stage lasts a different amount of time for each woman. It might last up to eight years, although it can also last only a year. Your body may begin to change during perimenopause as it adjusts to the new hormone levels.
While perimenopause marks the start of losing fertility, a woman undergoing this transition can still become pregnant. It is because perimenopause does not mean that the woman has stopped producing eggs. It just means that the woman produces fewer and less viable eggs. Some months, your ovaries may produce an egg, while in other months, they won’t. The implication is that it gets harder and harder to conceive. Perimenopause lasts until menopause occurs.
Perimenopause Vs. Menopause
It is usual to mistake perimenopause for menopause because, during this time, there is a possibility of going a few months without seeing a single menstrual cycle to completion. It might make many women believe they are experiencing menopause even when they are not.
Menopause is usually diagnosed retrospectively. For you to have gone through menopause, you must have gone an entire year or a period of 12 months without experiencing a complete menstrual cycle. The average age for menopause is 51, although some women have been known to experience menopause as early as 40 or as late as 55.
Menopause puts a stop to normal reproductive activities of the body. The hormone levels will not be strong enough to aid ovulation and childbirth. During this period, it is presumed that birth through natural means is no longer possible, and there isn’t a need for birth control. However, this is not the case for people still experiencing perimenopause. It is still possible, even if unlikely, for this group of people to conceive and carry a full-term pregnancy. So if that is not part of the plan, then birth control remains necessary even for people in this phase of their lives.
How To Increase The Chances Of Pregnancy During Perimenopause
This part of this article is for people going through perimenopause and are still hoping to give birth. And there might be many reasons people are in this phase of their lives. Some of these reasons could be:
- They were not ready for the responsibilities that came with childbirth, or they did not feel confident enough to see the process of childbirth through.
- It could be that they were not in stable situations, financially, mentally, or even physically, suitable for birthing a child.
- Finally, it could be the last hope for the woman trying to conceive for a long time.
We have mentioned before that it is possible to conceive during menopause. However, the possibility is very slim. Let us look at a few statistics.
- At age 38, 20% of women are incapable of conceiving naturally.
- This figure climbs to 50% by the time they are 41 and 90% when they are 45.
- By age 50, almost 100% of women find it impossible to conceive naturally.
It does not mean that these women are going through something ordinary. It just means that they are transitioning into menopause. And during this period, the quality and quantity of eggs they produce decreases until it is nonexistent. However, it is still possible to conceive during perimenopause because the ovaries can produce viable eggs. So on the rare occasion that they do this and this particular egg gets fertilized, it is still possible to carry this child for a full term and be a mother.
Increasing The Chances Of Getting Pregnant
While the statistics might seem bleak, it is still possible for a woman to get pregnant in the perimenopause phase of her life. Unfortunately, these chances are reduced, and the possibility of birthing a child during this time is slim. Women hoping to get pregnant during this period should discuss their options with their healthcare providers. However, we will list some ways a perimenopausal woman might increase her chances of giving birth.
- Monitoring Ovulation
Even when our reproductive clock is at its peak, it always helps track our ovulation. It is because targeting your most fertile window increases the chances of getting pregnant. There are ways, naturally and otherwise, to identify the best time to conceive. A few test strips and kits would help tell when it is best to attempt getting pregnant.
Some of the ways to measure these things include
- Calendar tracking where people with consistent menstrual calendars estimate that their ovulation would occur two weeks before their period begins. This method can get confusing as there are many things to consider when measuring your ovulation period. It is also not that dependable for people who have irregular menstrual cycles.
- Tracking Basal Body Temperature by taking your temperature first thing in the morning before getting out of bed. You’ve ovulated if your temperature rises for a long time. You can identify these temperature fluctuations by keeping a chart for the duration of your cycle. In some situations, BBT charting indicates whether or not you’ve conceived.
- Using ovulation predictor kits similar in use and functionality to the hormone pregnancy tests. They indicate an increase in the levels of luteinizing hormone. A marked increase in this hormone implies that ovulation will occur within the next 24 hours. After this, you are advised to have sex daily until ovulation has stopped. There are also digital fertility monitors that function the same way but offer more precision. The only drawback about these kits is that they tend to be pricey.
- Saliva testing is another way to detect ovulation. This type of testing is usually less expensive than ovulation prediction kits. There are chemical changes in the saliva during the most fertile stage of the menstrual cycle. When the residue is dried, it develops fern-like crystals absent in other cycle stages. A drop of saliva is placed on a lens in the test kit and examined under the viewing scope after about five minutes to determine if the typical chemical changes have occurred. Ovulation will likely occur within 24 to 72 hours following the initial forms.
- Cervical mucus charting is another way to get a good sense of when you’ll be ovulating. This monitoring method has good accuracy when utilized with basal body temperature charting. The cervical mucus thins and clears around the time of ovulation (the best time to have sex to conceive). It has a texture that is akin to raw egg whites. This weakening allows sperm to pass past the cervix during intercourse, allowing them to thrive in a more suitable alkaline environment.
- Diet and Exercise
When you’re trying to conceive, there’s a lot of advice on what to do and changes to improve your chances of getting pregnant. You may also have to improve on certain lifestyle adjustments to increase your chances of becoming pregnant.
Eating a well-balanced, nutritious diet and regular exercise improves overall health. It may raise the odds of conception. However, even if there was no scientific basis for this, having an overall healthy lifestyle does not come with disadvantages.
- In Vitro Fertilization
Advancements in technology have enabled perimenopausal women to conceive through assisted reproductive technology. One of the most popular procedures is in vitro fertilization. Unfortunately, during perimenopause, the chances of releasing viable eggs decrease, which is one of the major reasons the pregnancy rate among women in these phases is difficult.
Women who are well aware of this and want to conceive during their perimenopausal years would probably freeze their eggs to be able to use them when they can no longer produce viable eggs. However, it is still possible to get pregnant using donor eggs for women who did not have this foresight.
However, the chances of successfully conceiving and carrying a full-term child with these procedures decrease with age.
Risks Associated With Perimenopausal Pregnancy

Getting pregnant during perimenopause might fulfill a dear wish; however, these pregnancies come with risks or risks that have become more probable with age. For example, there is an increased risk of not carrying the full child term or delivering a clinically underweight child. The risks are even higher if the child is conceived through in vitro fertilization.
Other risks that increase with perimenopause pregnancy include:
- Fetal mortality or loss of the pregnancy before it is full-term.
- Preeclampsia presents as swelling of the limbs, proteinuria, and high blood pressure.
- A complicated delivery sometimes leads to the need for cesarean delivery.
- Issues with the health of the mother.
- An increased probability of giving birth to a child with congenital abnormalities.
Individual risks might also arise due to personal medical issues. A healthcare professional is in the best position to handle all these concerns.
Is Pregnancy Possible During Menopause
Now that we have discussed the possibilities of getting pregnant during the transition to menopause, the next question would be, “Is it possible to get pregnant during menopause?” and the short answer would be “Yes! It is indeed possible to get pregnant during menopause. It is a feat that has been achieved by many people, as we will see later on in this article, but before that, let us look at the science behind this assertion.
As of the time of writing this article, it has not changed that once a woman has gone through menopause, their hormone levels have become so low that they are incapable of releasing more eggs for fertilization. It simply means that a woman cannot get pregnant naturally.
A woman has two biological clocks. There is an ovarian clock that works until menopause and stops. At this point, the woman cannot produce any viable egg. However, there is another clock, the reproductive clock, and this one goes even after the ovarian clock has stopped. The implication is that a woman undergoing menopause might be able to produce eggs. However, their body can still carry a fertilized egg and give rise to a baby. And with all the advancements in technology, this is possible.
Technology in medicine keeps breaking through the natural barriers to pregnancy. Before, once someone enters perimenopause, they won’t be able to get pregnant or carry a full child to term. But with each passing year, new procedures and old ones are improved. Right now, a woman in their late 50 can carry a full child to term and deliver a healthy baby.
All required is some hormone priming (estrogen and progesterone), followed by a healthy, fertilized egg supplied by someone else. There are predicted adverse effects, including the risk of Cesarean Sections; nevertheless, these side effects are usually bearable enough that a 50- or 60-year-old woman should not rule out pregnancy completely.
So what does this mean for the menopausal woman who wants to bear a child? While they can’t produce a viable egg for fertilization, advancements in medical technology have made it possible for women to carry and birth a child, and we will be looking at the possible ways they can achieve this.
Options Available For Menopausal Women Who Want To Get Pregnant
So since we have established that menopausal women can give birth, let’s talk about how they can achieve this. In medicine, there has been a lot of research into how women having fertility issues can conceive and carry a child full-term. These methods are known as assisted reproductive technology.
It encompasses all the possible ways eggs and embryos are handled for fertility therapy. ART treatments entail surgically extracting eggs from a woman’s ovaries, mixing them with sperm in the lab, and either returning them to the woman’s body or transferring them to another woman for fertility. Artificial insemination and ovary drug therapy are not considered part of assisted reproductive technology.
The most common form of these procedures is in vitro fertilization (IVF). Assisted reproductive technology has a very high success rate, with 6.5 million children successfully delivered using this method.
An Overview Of In Vitro Fertilization
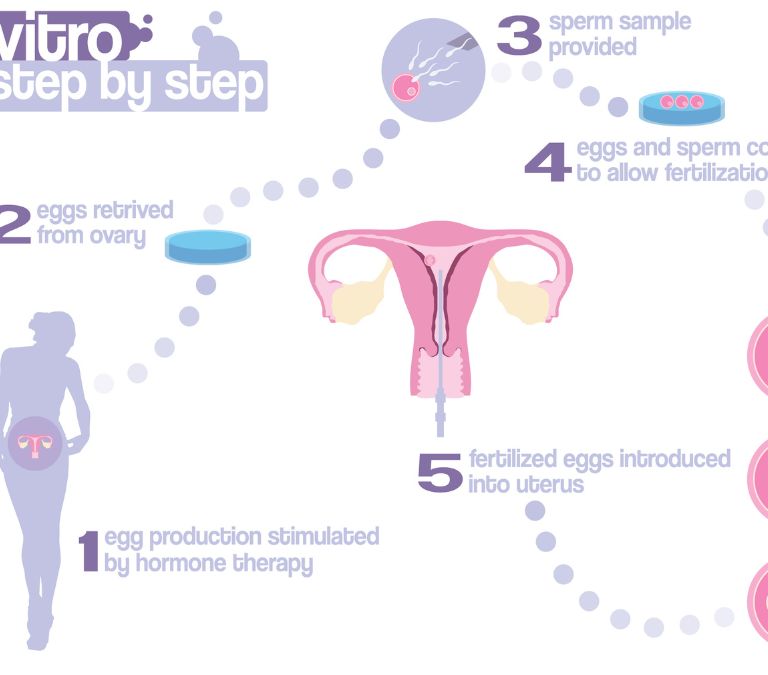
Biologically, for a pregnancy to occur, a woman must produce a viable egg during ovulation. This egg is penetrated by a sperm cell from a man, and fertilization occurs. After this, the fertilized egg attaches to the uterus wall, and a baby starts to develop.
But for women undergoing menopause, the ovulation process does not occur. Hence, there is no viable egg to fertilize; hence unassisted or natural conception can’t occur. It is where in vitro fertilization as a treatment option comes into play.
Depending on the situation, in vitro fertilization uses the frozen eggs of the menopausal woman, if she had the forethought to do that or fresh/frozen eggs from a donor. In vitro fertilization for menopausal women is done in four steps if a donor is included.
- Stimulation
The egg donor takes fertility drugs to produce multiple eggs. During each menstrual cycle, a woman generally produces one egg. IVF, on the other hand, necessitates the use of several eggs. The chances of producing a viable embryo increase when many eggs are used.
The woman is given reproductive medicines containing the follicle-stimulating hormone (FSH). FSH causes the ovaries to generate more eggs than they normally would. The doctor will conduct routine blood tests and ultrasounds to check egg production and determine when to retrieve the eggs.
- Retrieval Of Eggs
Follicular aspiration is a small surgical operation used to collect eggs. A very thin needle is introduced into the ovary through the vaginal canal. The needle has a suction device attached to it. The eggs are sucked out as a result of this. Each ovary goes through the same procedure.
According to studies, extracting 15 eggs from the ovaries in a single cycle increases the chances of a healthy pregnancy.
- Insemination and Fertilization
The semen sample from the male partner will be mixed with the eggs that have been aspirated and kept in a closely controlled environment. It will cause the sperm to penetrate the egg and fertilize it. Another way to achieve this would be to inject the sperm cell directly into the egg through an intracytoplasmic sperm injection (ICSI).
Once fertilization occurs, the egg divides, and an embryo is formed. Then, the embryos are examined, and a couple of the most viable embryos are prepared for transfer.
- Embryo Transfer
When the embryos are ready for transfer, they are implanted into the woman’s uterus. It usually takes place a few days after the fertilization of the eggs. This process involves passing a catheter into the uterus and planting the fertilized eggs, through the catheter, into the uterus. The woman is deemed pregnant within 10 days if the embryo successfully attaches itself to the uterine wall.
The process of in vitro fertilization comes with cons and complications. First, it is a very expensive procedure. Most people consider it a last resort because of how invasive and stressful it is. For women undergoing menopause, however, there aren’t too many options, so they have to bear the risks that come with it. We will dwell on these complications later on in this article.
First, however, you must remember that the success rate of in vitro fertilization declines with age, like every other fertility treatment. According to the American Pregnancy Association statistics, women under 35 who undergo IVF have a live birth rate of 41 to 43 percent. For women older than 40, the percentage drops to 13 to 18 percent.
Ovarian Rejuvenation
This relatively new procedure is still in the experimental phase, but we thought it wise to mention it here. The premise is that it is scientifically possible to rejuvenate ovaries that are no longer functional. It is done by using growth factors in the woman’s platelet-rich plasma. It will cause the development and release of viable eggs for fertilization. This process is called PRP therapy for ovarian rejuvenation.
Successful Cases of Menopausal Women Who Got Pregnant.
As we have already mentioned, getting pregnant and carrying a child full-term during menopause is possible. In addition, there are cases of people who had gone through assisted reproductive technology when all hope seemed to be lost, and they managed to conceive and carry a full pregnancy to term.
One memorable case is that of 70 years old Maldhari, who got pregnant through in vitro fertilization after trying to get pregnant for 45 years. In the past, it would have been virtually impossible to get pregnant and bear a child at 70. Still, with the advancement of technology, it has become possible. Maldhari’s case is not an isolated one. There have been several success stories about menopausal women who give birth through assisted reproductive technology.
There is the case of Mangayamma, who gave birth to twin girls through in vitro fertilization at the age of 74. This event created a buzz in medicine as it was considered a literal medical miracle. Another case of notable success in vitro fertilization is the case of Naomi Campbell. The famous supermodel got pregnant at fifty through assisted reproductive technology. These successes are just a few of the 6.5 million cases that have been reported.
Recently, there has been further development in this field as women who were thought to have reached the end of their ovarian clocks managed to get pregnant with eggs produced by their ovaries. It was accomplished using platelet-rich plasma therapy.
At least two pregnancies have been recorded, and the women were already experiencing menopausal signs in these two cases. Although this is a fairly new development and is still under experimentation, the results seen so far are promising. They might bring a breakthrough that will make its way into the pages of history.
Health Risks Faced By Women Who Get Pregnant After Menopause
It is no longer uncommon to see women get pregnant during the menopausal transition; with the advances in assisted reproductive technology, the success rates of these pregnancies have and will continue to increase. However, this does not mean there are no risks associated with pregnancies at this age.
The risks associated with pregnancies increase with age, and the changes brought about by menopause also cause an increase in these risks. Let us look at some of the risks associated with getting pregnant through natural means or IVF during the menopausal transition.
Genetic Risks
As women get older, certain genetic risks become increasingly prevalent in pregnancy. The likelihood of having a kid with Down syndrome, for example, increases with maternal age.
At the 10th week of the pregnancy, the chance of an embryo having Down syndrome is 1 in 1,064. It rises to 1 in 686 at age 30 and 1 in 240 by age 35. At 40, the Down syndrome rate rises to 1 in 53 embryos, then drops to 1 in 19 embryos at 45.
A recent study aimed to discover why older moms are more likely to produce infants with congenital abnormalities characterized by aberrant chromosomal numbers. Researchers discovered that genetic recombination might be responsible for the higher likelihood of disorders like Down syndrome.
Recombination is the exchange of genetic material between chromosomal pairs before they separate. The researchers discovered that the recombination process is less regulated in older moms, resulting in aberrant chromosome counts in sex cells or massive chromosomal rearrangements.
Miscarriages and Stillbirths
As the mother’s age rises, so does the risk of miscarriage. According to current studies, the likelihood of miscarriage is around 8.9% for women aged 20 to 24 and 74.7% for those aged 45 and up. The increasing rates of miscarriage are assumed to be due to the deteriorating quality of women’s eggs.
Stillbirth is also more common in older women and women who have reached menopause than in younger women. Due to the higher risk of stillbirth in women over 35, they are commonly advised to be induced as their due date approaches.
The reasons for the increase in stillbirth rates as mothers get older are unknown.
Multiple Births
It’s also more likely to have twins or triplets as you age, especially if you use IVF.
Transferring more than one embryo into the womb increases the chances of conceiving twins, triplets, or more infants.
Preterm birth or low birth weight can occur in multiple-fetus pregnancies and a twofold increase in the mother’s chance of developing diabetes and a considerable increase in the mother’s blood pressure.
There you have it. Everything you need to know about pregnancy during the menopausal transition: fertility and reproduction does not have to come to an end just because a woman becomes menopausal, and while it is very easy to give up hope of birthing children once the symptoms of menopausal transition start showing, there is still that possibility of giving birth even after menopause.
Even during the postmenopausal period, the possibilities of conceiving and bearing a child have been improved upon by advancements in medicine. If you are experiencing menopause and still want to give birth, talk to your healthcare provider to consider the available options.







